Lichen Planus
Lichen planus is a rash that affects the skin and, less often, the scalp, fingernails, toenails, and/or inside the mouth or genital area (mucous membranes). Lichen planus can resolve on its own without treatment, or it can be persistent, even with aggressive treatment.
Who's At Risk?
People of any age, race / ethnicity, and sex can have lichen planus. However, it is rarely seen in young children and older adults; it is most common in people aged 30-60.
Although the cause of lichen planus is unknown, some people with the condition also have hepatitis C, an infection of the liver.
People who take certain medications may develop drug-induced lichen planus. These medications include:
- High blood pressure (hypertension) medicines, including diuretics (eg, hydrochlorothiazide), ACE inhibitors (eg, lisinopril), and calcium channel blockers (eg, nifedipine).
- Diabetes medications, including sulfonylureas.
- NSAIDs such as ibuprofen (Advil, Motrin) and naproxen (Aleve).
- Antimalarial medications.
- Penicillamine.
- Tumor necrosis factor (TNF)-alpha inhibitors.
- Tyrosine kinase inhibitors.
Signs & Symptoms
The most common locations for lichen planus include the:
- Inner wrists.
- Forearms.
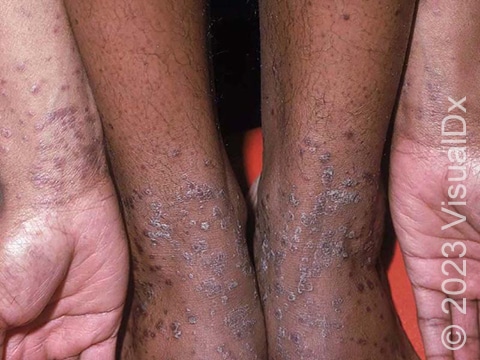
- Inner ankles.
- Lower legs.
- Neck.
- Trunk.
- Mouth.
- Fingernails and toenails.
- Scalp.
- Genitals.
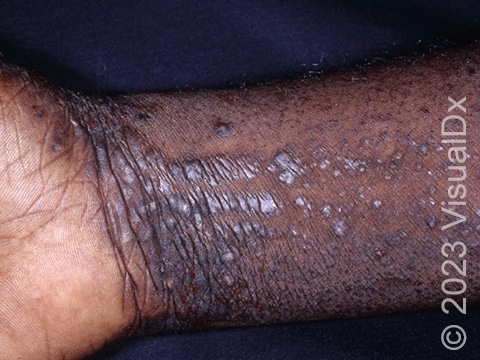
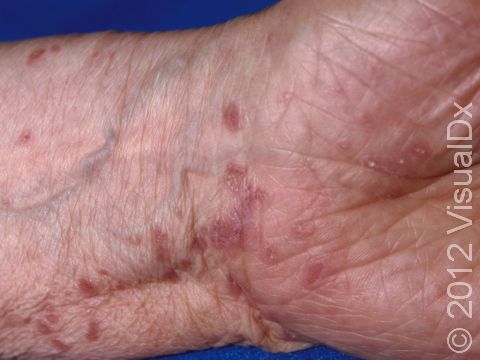
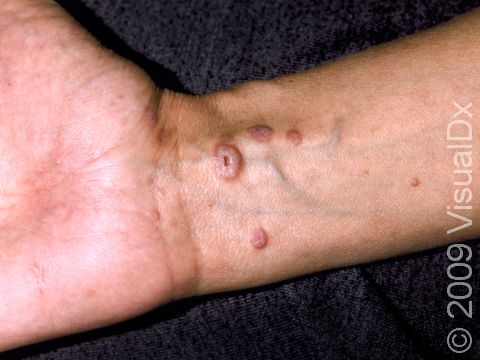
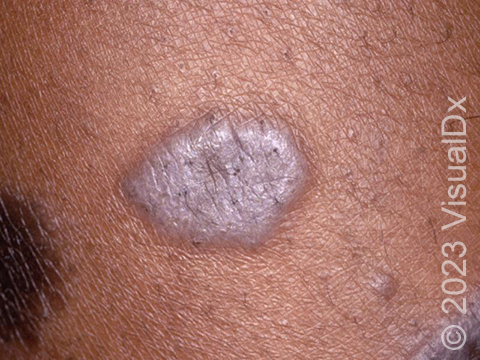
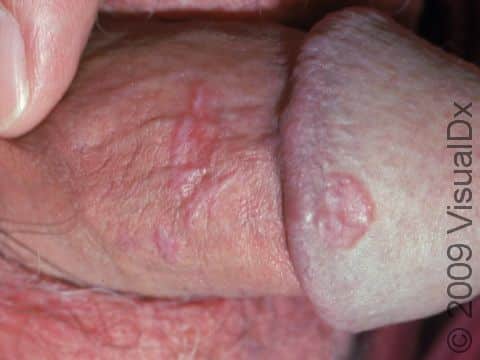
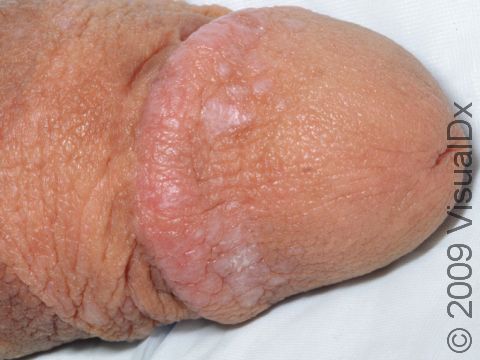
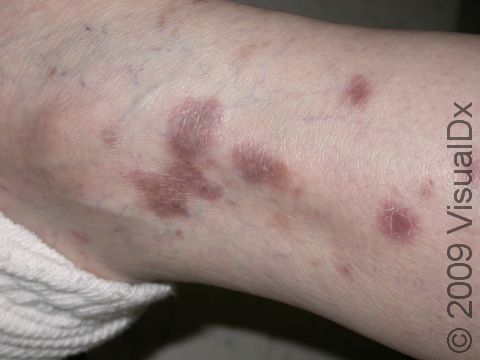
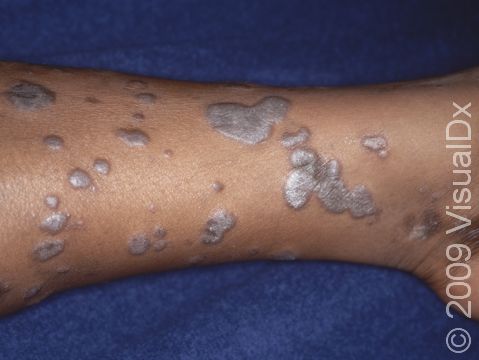
Lesions of lichen planus on the skin appear as small, flat-topped, solid bumps (papules) and larger flat-topped, raised areas larger than a thumbnail solid (plaques). In lighter skin colors, the lesions are often pink, red, or purple. In darker skin colors, the lesions are often dark purple or gray. As lichen planus progresses, the surface of these bumps can become dry and scaly and can develop wispy, gray-to-white streaks (called Wickham’s striae). Lichen planus on the skin is usually itchy.
New lesions of lichen planus can be caused by injury to the skin.
Once lichen planus lesions heal, they often leave behind patches of dark gray skin, which are more pronounced in darker skin colors. These areas may take months to return to their normal color.
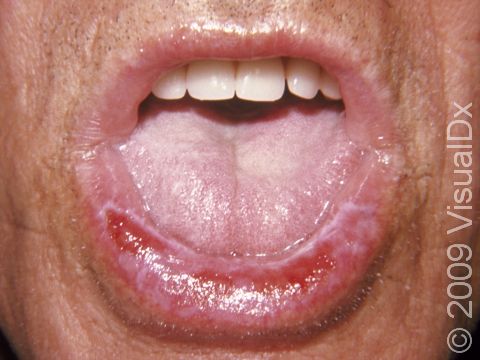
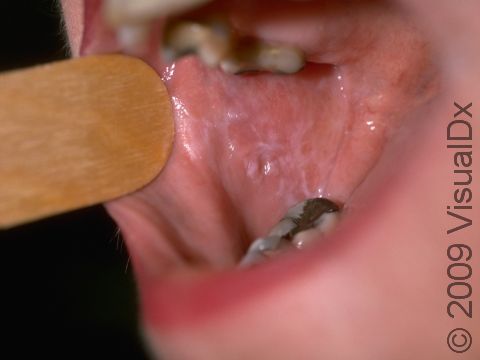
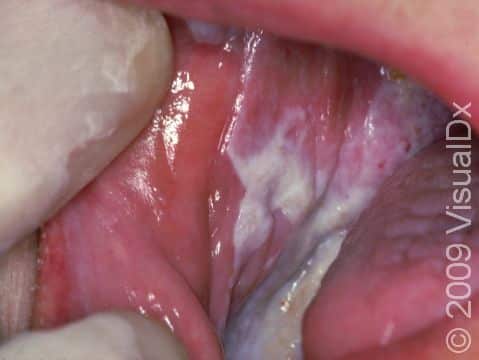
In the mouth, lichen planus appears as white streaks or patches (flat, smooth areas that are larger than a thumbnail), most often seen on the inner cheeks. Oral lichen planus is usually not painful, but in severe cases, there may be painful sores in the mouth.
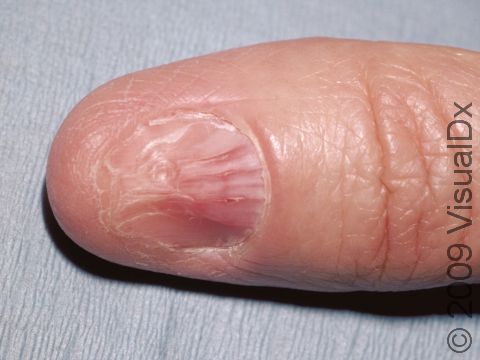
When lichen planus involves the fingernails or toenails, the nails may become thick, or they may have splitting, ridges, or grooves. In severe cases, the entire nail may be destroyed.
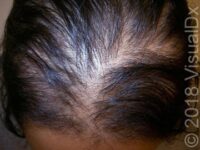
On the scalp, lichen planus (called lichen planopilaris) may cause skin color change, irritation, and, in some cases, permanent hair loss.
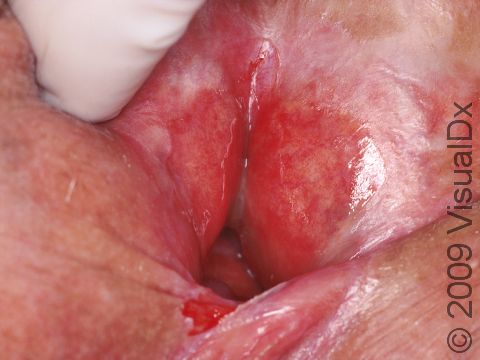
On the genitals, lichen planus lesions may be quite tender and sores may develop, especially in women.
Self-Care Guidelines
- Apply over-the-counter hydrocortisone cream to help relieve skin itching in mild lichen planus.
- If you have lichen planus in the mouth, avoid drinking alcohol and using tobacco products.
Treatments
Your medical professional will check your medication list to see if one of your medications may be the cause. If lichen planus is suspected, a dermatologist may want to perform a skin biopsy.
In addition, one of the following treatments may be recommended:
- Topical corticosteroid cream, lotion, ointment, or gel, eg, prednisone (Rayos), betamethasone (Diprolene, Celestone), triamcinolone (Aristospan, Kenalog), or Halobetasol (Ultravate, Halonate)
- Corticosteroids injected directly into any thick lesions
- Oral antihistamine pills such as loratadine (Claritin), cetirizine (Zyrtec), fexofenadine (Allegra), desloratadine (Clarinex), hydroxyzine (Vistaril), or diphenhydramine (Benadryl) for itching
- Ultraviolet light treatment
- Topical tacrolimus (Protopic) or pimecrolimus (Elidel)
In the case of oral lichen planus, the medical professional may suggest one of the following:
- Topical corticosteroid mouthwash, ointment, or gel
- Pain-relieving mouthwash
For severe cases of lichen planus, one of the following therapies may be recommended in addition:
- Oral medications, such as prednisone, metronidazole (Flagyl), isotretinoin (Amnesteem, Claravis), acitretin (Soriatane), and hydroxychloroquine (Plaquenil)
Although there is no cure for lichen planus, treatment can usually minimize symptoms and improve the appearance of the rash until it heals.
Visit Urgency
If you develop an itchy, bumpy rash, see a dermatologist or another medical professional for evaluation.
If you have severe oral lichen planus, there is a very small chance of developing oral cancer, so you should see your dentist twice a year to check for cancer.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 26th, 2024 at 11:00 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder