Heat Rash or Prickly Heat (Miliaria Rubra)
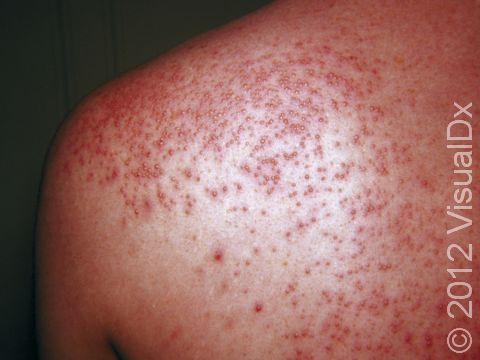
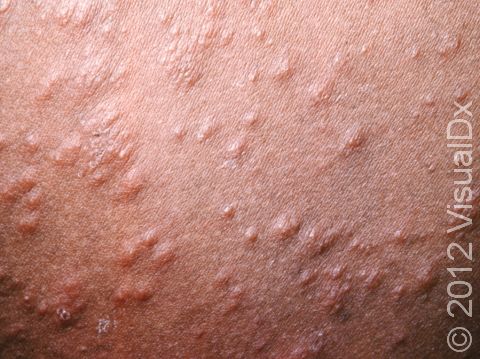
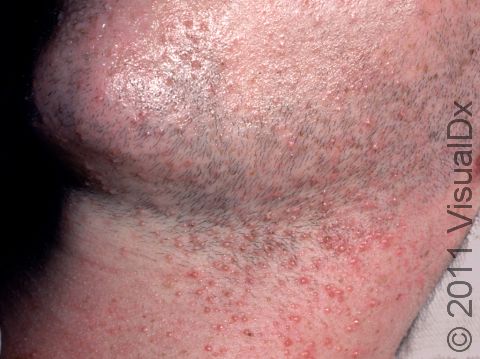
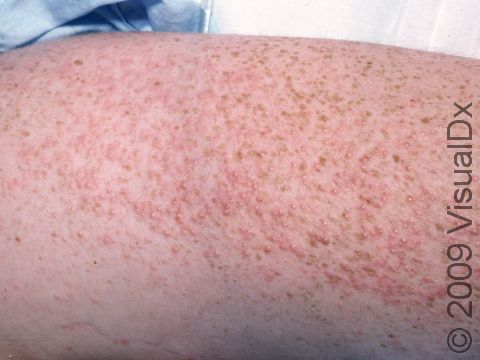
Miliaria rubra, commonly known as heat rash or prickly heat, is a rash caused by blockage of the sweat ducts that carry sweat from sweat glands to the skin surface. It can cause discomfort, itching, and sometimes a stinging or prickly sensation.
Who's At Risk?
Heat rash is more common in hot, humid climates. Anyone who is new to such an environment is especially vulnerable. Heat rash can be due to high fever, excessive sweating, or being overly bundled. In adults, heat rash commonly occurs in areas where blockage of sweat ducts occurs, such as the back in people on bed rest, the neck, the trunk, and body folds, where there is skin-on-skin contact.
Signs & Symptoms
Heat rash commonly occurs after exposure to hot conditions. There can be many small, red papules (solid bumps) all over the body on a base of red skin. In darker skin colors the redness may be harder to see or may look more purple. Heat rash usually occurs on skin that is covered or where there is a lot of friction, such as the neck, chest, and body folds. The face, palms, and soles are generally not affected by heat rash. The rash can cause intense itching and stinging, which can become worsened by heat. You may feel fatigued and become intolerant of heat due to little or no sweating at the affected areas.
Self-Care Guidelines
Prevention and treatment of heat rash consists of controlling heat and humidity.
- Try to maintain a cool environment, such as going to an air-conditioned space, applying cool compresses, or taking a cool shower or bath.
- Wear loose-fitting clothing.
- Drink plenty of fluids.
- If the rash is itchy, an oatmeal bath or calamine lotion may help.
- Try to rest and avoid overexertion, especially in hot weather.
- Avoid applying any heavy moisturizers to the skin.
- In the case of fever, taking acetaminophen (Tylenol) or ibuprofen (Motrin, Advil) can help.
Treatments
Your medical professional may prescribe a topical steroid lotion or cream to help with symptoms.
If there are signs of secondary bacterial skin infection associated with the heat rash or otherwise, oral or topical antibiotics may be given.
Dehydration may be treated with intravenous fluids, especially if there is vomiting. Heatstroke is treated by trying to quickly reduce the core temperature to normal. Immersion, evaporative, or invasive cooling techniques may be used in addition to rapid administration of intravenous fluids. This type of care is administered within a hospital setting.
Visit Urgency
Typically, heat rash will resolve with self-care measures and no medical care is necessary. However, two complications from heat rash include secondary infection from scratching and heat exhaustion.
Although uncommon, infected areas due to breaks in the skin caused by scratching may need antibiotic treatment for resolution. Seek care if the rash develops pus, redness, crusting, swelling, or tenderness.
In cases of heat exhaustion, the skin will appear hot and flushed without any sweat. The person may complain of dizziness, nausea, weakness, headache, confusion, or difficulty breathing. Heat exhaustion can progress to heatstroke, so seek urgent medical care. Symptoms of heatstroke include a very high temperature of 105°F (40.56°C) or greater, decreased or loss of consciousness, or seizure.
While awaiting medical care, get the affected person indoors or under shade, undress them, and apply cool compresses to the body.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 18th, 2024 at 8:48 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder