Head Lice (Pediculosis Capitis)
Head lice infestation (pediculosis capitis) is a common highly contagious infection that often occurs in nurseries, day-care centers, and schools. It is caused by infestation with the human head louse, and it is usually very itchy.
Lice are very small insects that feed on human blood. The female louse attaches her eggs (nits) to the base of the hair, near the scalp, and the nits hatch 7-10 days later. While the adult louse cannot survive for more than 2 days off the human head, a nit can stay alive for up to 10 days off the body (such as on clothes, hairbrushes, and carpets). Lice are spread by close head-to-head contact and by sharing belongings that are infested with lice.
Who's At Risk?
Head lice can occur in anyone, but children aged 3-11 years are most likely to become infested. All socioeconomic groups can be affected, and infestation is not related to the cleanliness of the person or their environment. Because the louse’s claws are better able to grasp certain hair types more than others, those with coarse, curly hair are affected less often than those with straighter hair types. In addition, girls are more likely to have head lice than boys, as longer hair will lead to more instances of hair-to-hair contact. Head lice infestations are most often seen in situations in which there is close personal contact, such as schools, home, playgrounds, sports, and camp. Human head lice eat only human blood, so pets and other animals do not spread the infection.
Signs & Symptoms
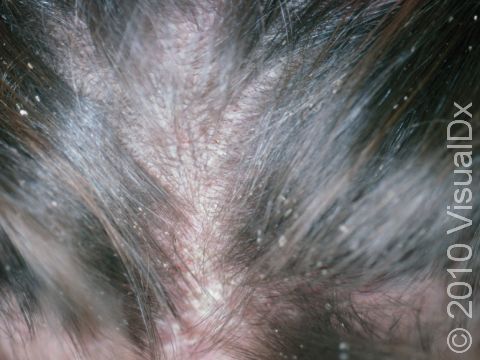
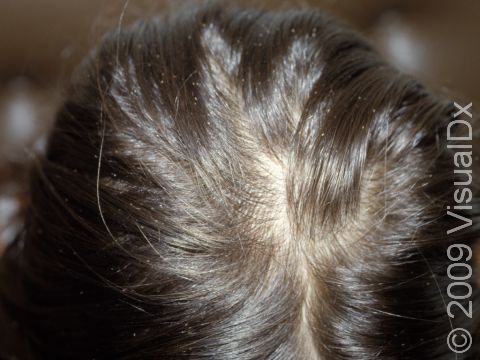
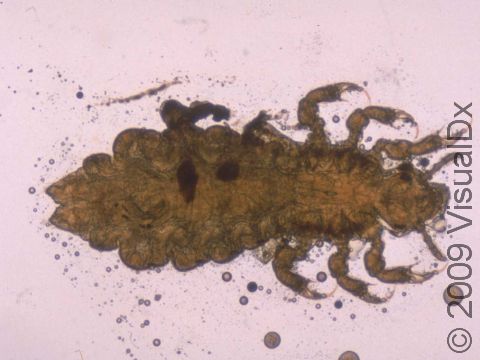
The earliest sign of infection is itching of the scalp. You may see your child scratching their scalp a lot. Lice and nits may be seen on the scalp and hair. Each louse is approximately 1-3 mm long and has 3 pairs of claw-like legs. Lice crawl; they do not jump or fly. Nits are smaller, about 0.5-1 mm, white-gray, and are firmly attached to the hair close to the scalp.
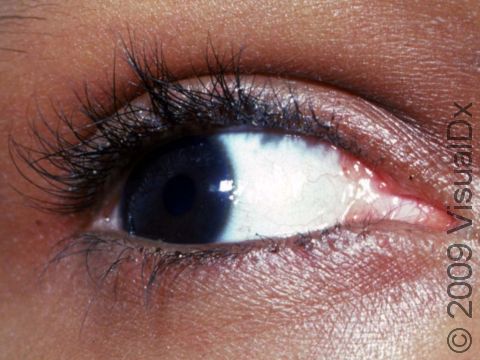
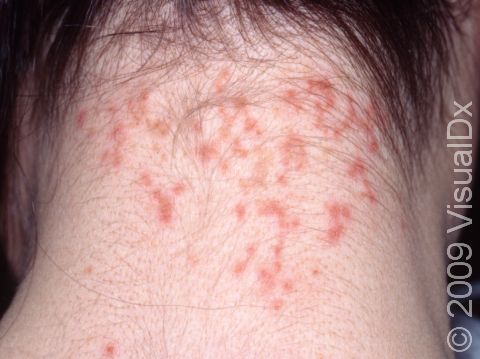
Small bumps that are red or darker than the surrounding skin may be seen on the scalp, neck, and shoulders. Occasionally, the lymph nodes behind the ears or in the neck may be swollen and tender. Lice may sometimes be seen on the eyelashes, causing the eyes to become red and irritated.
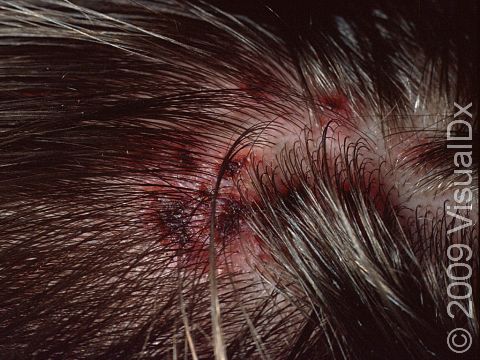
Because head lice infestations are itchy, scratching is common and may lead to resultant infection or scabbing. In addition to an itching or tickling sensation, children may also be irritable or have difficulty sleeping.
Self-Care Guidelines
In early infections, it may be difficult to spot the lice and nits. If you think your child may have head lice, search for lice and nits using a fine-toothed comb, also called a louse comb, that can be purchased at most drug stores. Examine your child’s scalp with a bright light, and use a magnifying glass if necessary.
If you find lice and/or nits, follow these guidelines:
- Over-the-counter medications for head lice are typically effective and include pyrethrins (eg, A-200, Pronto, R&C, RID, Triple X) and permethrin lotion 1% (Nix). These medicines kill only live lice, not the eggs, so reapply the medication in 7-10 days to kill newly hatched lice. These treatments are only minimally absorbed through the skin, but they should not be used on children aged younger than 2 years. Ivermectin (Sklice) lotion is approved for ages 6 months and older. Use the medication exactly as directed. These medicines are insecticides and should not be applied in a larger quantity or more frequently than recommended.
- Before applying the medication, do not use conditioner on the hair, as this will coat the hair and protect the lice from the medicine. Use a nit comb after application. Also, do not wash the hair for 1-2 days after treatment.
- Another option is mechanical treatment. This means that all nits and lice are manually removed with a nit comb. This will require meticulous attention to detail and is time intensive. This process should be repeated at least weekly for 3 weeks to ensure all live nits and lice are removed. Professional lice and nit remover services may be available in your geographic area, but these services are costly.
- After treatment, wear clean clothes and wash other clothes, bed linens, and towels in hot water (hotter than 130°F [54.45°C]) and dry them using the hot cycle for at least 20 minutes.
- Wash all washable objects your child has been in contact with during the past 48 hours in hot water for at least 5 minutes.
- Seal potentially contaminated nonwashable objects in plastic bags for 2 weeks. (The lice will die within 2 days, and the nits will hatch and die within 2 weeks.)
- Vacuum floors and furniture.
- Examine the hair and scalp of household members and treat them if they are infested.
- Notify the school nurse, teacher, or day-care provider if your child has head lice.
- Do not share combs, hairbrushes, hats, towels, bedding, clothing, headphones, stuffed toys, or other items with someone who has head lice.
Treatments
To diagnose head lice, the medical professional will look for a louse or a nit on the scalp. They may shine a black light at the scalp called a Wood’s lamp, as the insects and eggs appear as fluorescent yellow-green spots under this light.
If the medical professional confirms your child has lice and you have not yet treated the infestation, they will likely recommend over-the-counter medications as described in the Self-Care Guidelines section. If you have already used over-the-counter medications and you still see moving lice, the medical professional will likely recommend a prescription-strength medication. These include the following:
- Permethrin – in children ages 2 months and older
- Malathion lotion (Ovide) – in children ages 6 years and older
- Spinosad cream (Natroba) – in children ages 4 years and older
- Ivermectin pills (Stromectol) – in children who weigh 33 pounds or more
Visit Urgency
See your child’s medical professional if you have any questions about self-care measures or if you continue to see crawling lice 8-12 days after treatment. Your child may need retreatment with a different medicine. Also call a medical professional if you notice any signs of bacterial infection on the child’s scalp, such as redness, swelling, pain, or pus. If you are pregnant, consult a medical professional to discuss the risks of using lice treatments.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 14th, 2024 at 1:02 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder