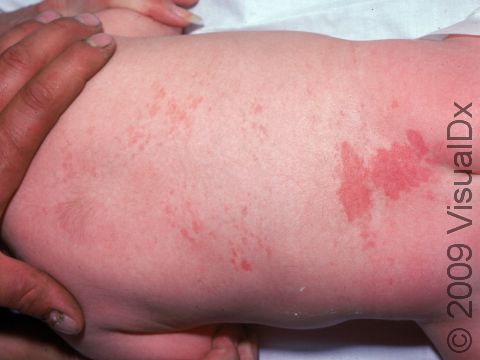
Port-Wine Stain
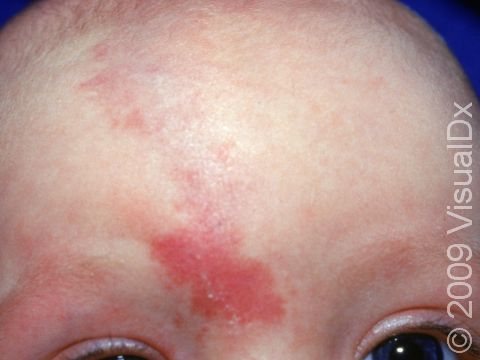
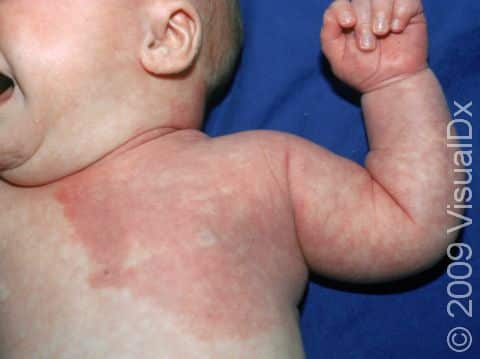
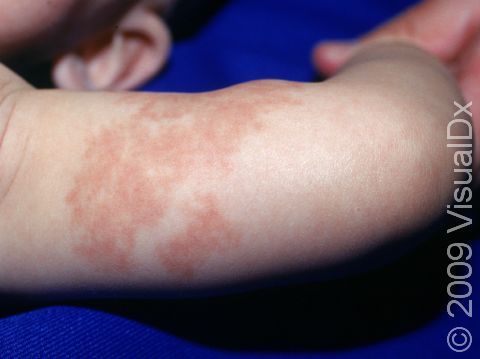
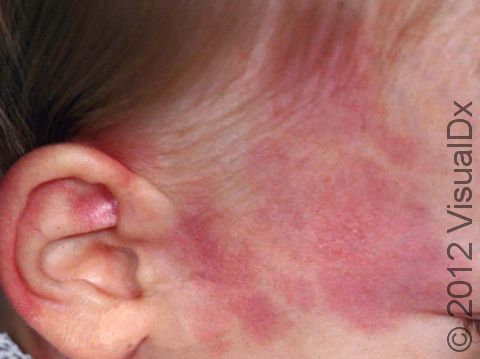
Port-wine stain, also called nevus flammeus, is a common permanent birthmark that is caused by a malformation of tiny blood vessels called capillaries. Port-wine stains are described as looking like spilled red wine on the skin.
Port-wine stains are flat at first, but with time, they may become raised. Their color may also deepen over time, starting off as a light red color and becoming deeper red, maroon, or purplish. Usually port-wine stains occur on their own and are harmless, but sometimes they may be a presenting sign of a syndrome. For example:
- Sturge-Weber syndrome involves a port-wine stain on the forehead and eyelid on one side of the face. It affects the brain on the same side as the birthmark and sometimes other body organs, such as the eye.
- Klippel-Trenaunay syndrome involves a malformation of the veins, a port-wine stain, and excessive growth of the soft tissues. Some individuals with this syndrome have one limb that is longer and larger than the other limb.
- Phakomatosis pigmentovascularis is the coexistence of a vascular birthmark (such as a port-wine stain) and pigmentary birthmark (such as a mole). It may affect the skin only or may also involve the brain, eyes, and/or musculoskeletal system.
- Port-wine stains on the lower back may be associated with spinal cord abnormalities.
Who's At Risk?
Approximately 1 in 1000 babies are born with a port-wine stain. There is no known association within families (genetic tendency).
Signs & Symptoms
Port-wine stains are always present at birth, and initially they appear as a flat, irregular patch (an area of skin larger than a thumbnail) that is pink or light red. They often change in appearance as the baby gets older and grows. The color will deepen and become darker red or purple, and the patches become thicker and have more of a cobblestoned appearance. Port-wine stains are not painful or itchy. It is sometimes difficult to tell the difference between a port-wine stain and other birthmarks, such as a salmon patch or a hemangioma, but it can be diagnosed by your child’s medical professional based on its appearance.
Self-Care Guidelines
Treat the port-wine stain as you would any other skin on your baby, with careful, gentle cleansing and moisturization.
Treatments
For treatment of the port-wine stain, your child’s medical professional may advise you to wait and see how the patch develops. There is no treatment necessary for a port-wine stain, but if the appearance is a concern, it is more effective to begin treatment earlier rather than later. The treatment usually involves laser therapy of the skin. Further testing to make sure that there are no associated syndromes that involve the brain or the baby’s development may also be recommended.
Visit Urgency
If your baby has a port-wine stain, see their medical professional, who may want to do further testing to rule out an associated syndrome.
If your baby’s skin bleeds or develops cracks or other problems, contact their medial professional for further advice.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 14th, 2024 at 3:50 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder