Acne (Acne Vulgaris)
Acne, also known as acne vulgaris, is a common skin condition that affects people of all ages, but it is especially common in teens and young adults.
Acne is often hereditary, meaning it runs in families. While there is no cure for acne, almost all acne can be improved by simple measures and treatments your doctor can recommend. Many people are bothered by their acne and are embarrassed to talk about it, but it is very important to discuss it with your doctor because they will be able to give you tips and prescribe products that can make a big difference.
Acne can result in scarring, so minimizing breakouts and avoiding picking at the skin is important.
Who's At Risk?
Acne affects 85%-100% of people at some point in their lives, and it usually begins at puberty. Most people have acne in their teen years that goes away by adulthood. However, acne can persist into the 30s and beyond, and some adults who never had acne as a teen can develop acne for the first time. It is estimated that 5% of people older than 45 have acne. People of all races / ethnicities get acne.
Signs & Symptoms
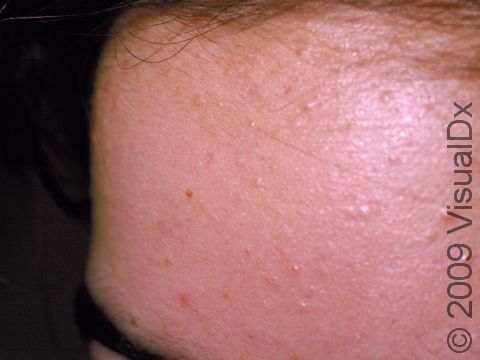
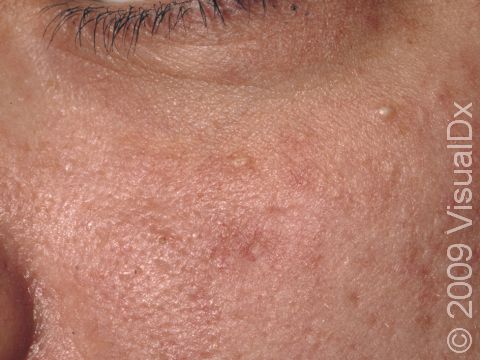
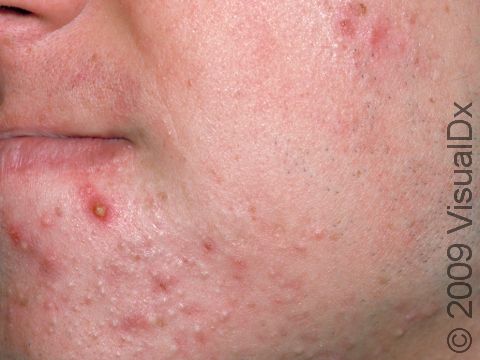
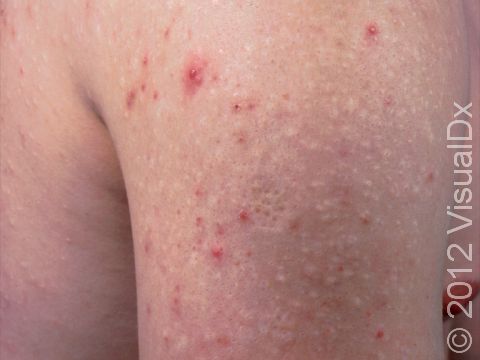
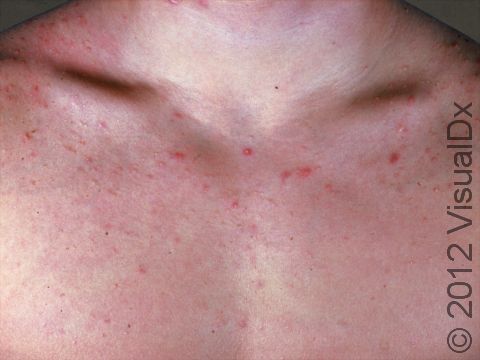
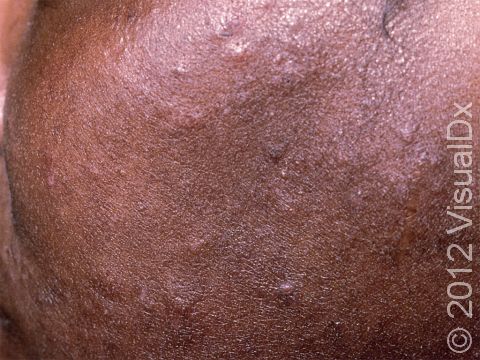
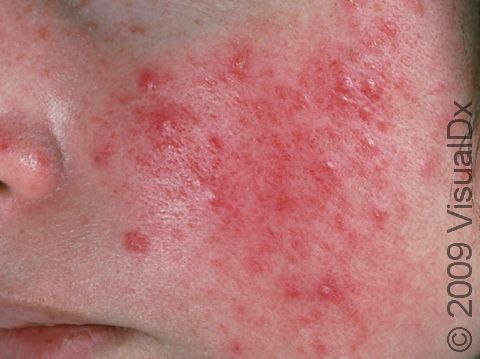
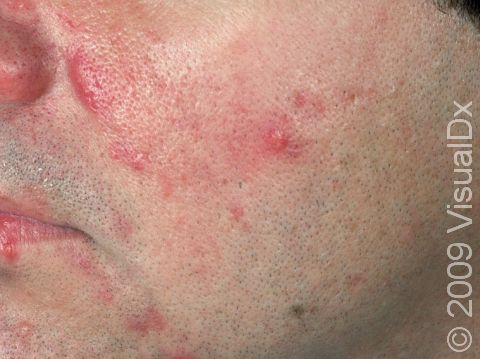
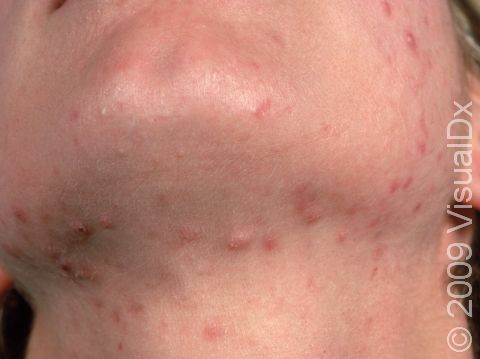
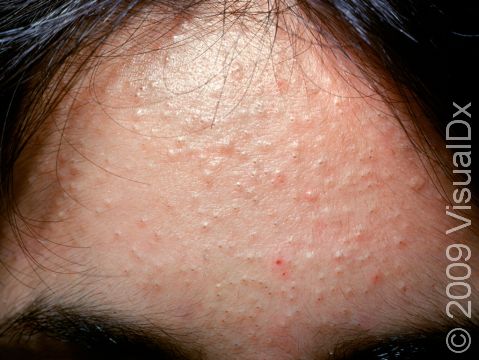
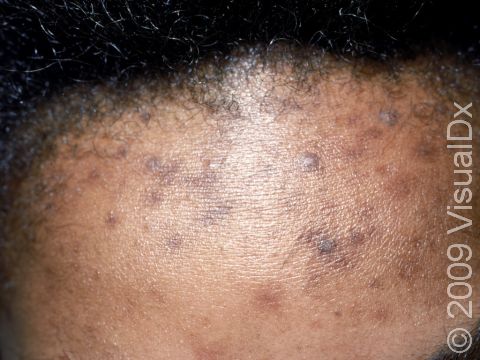
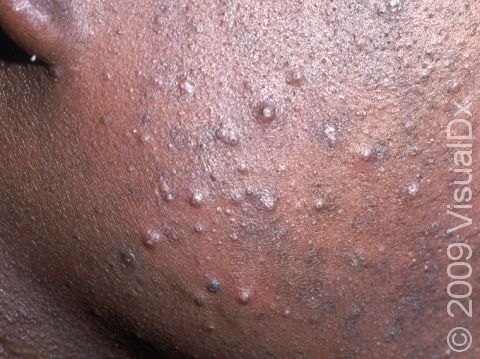
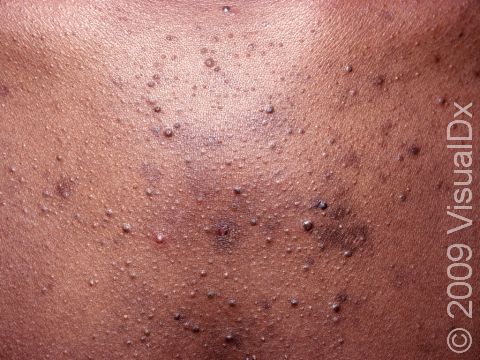
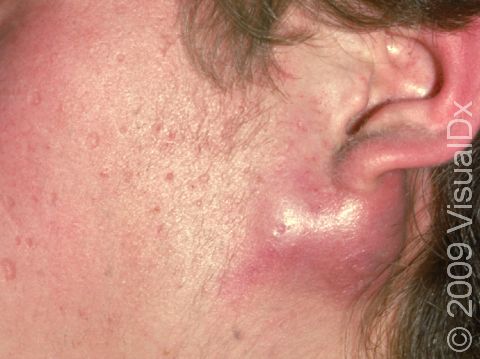
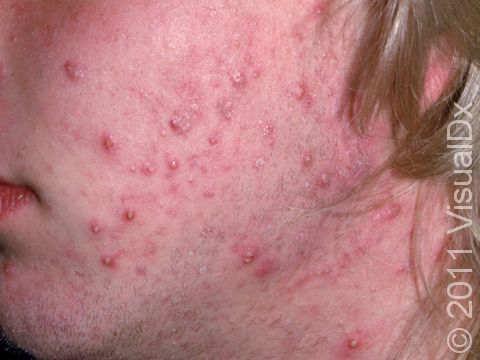
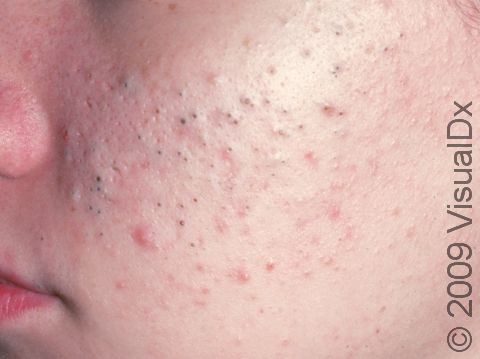
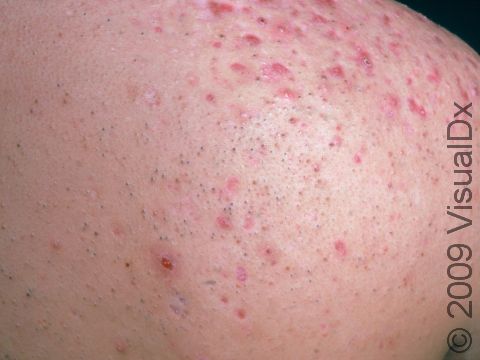
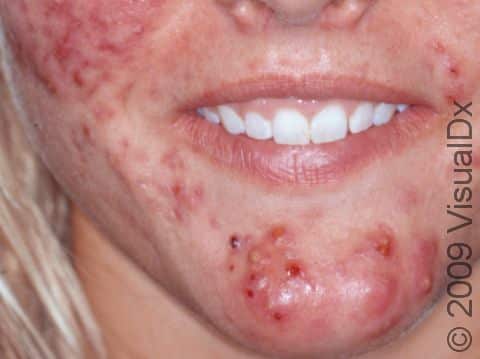
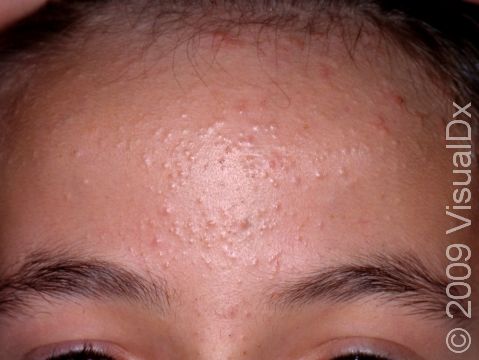
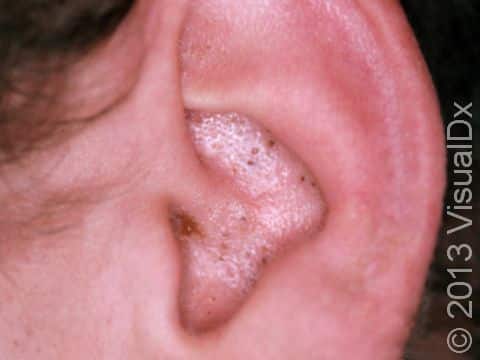
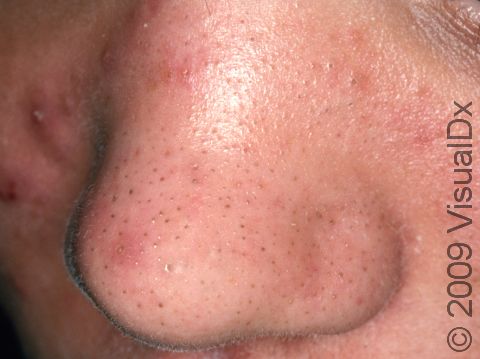
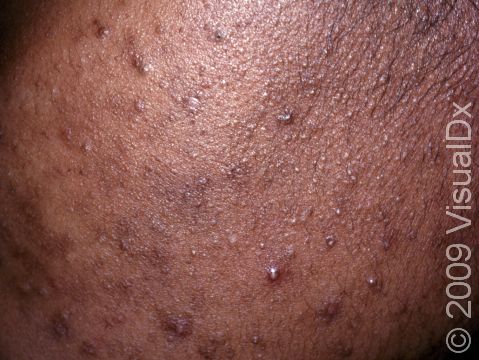
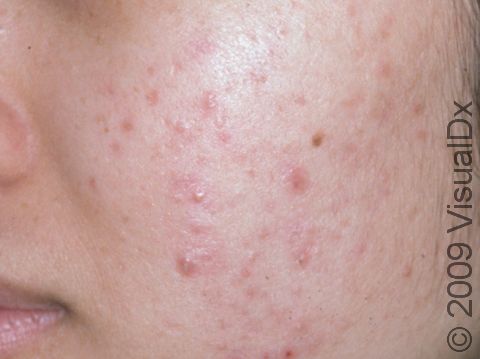
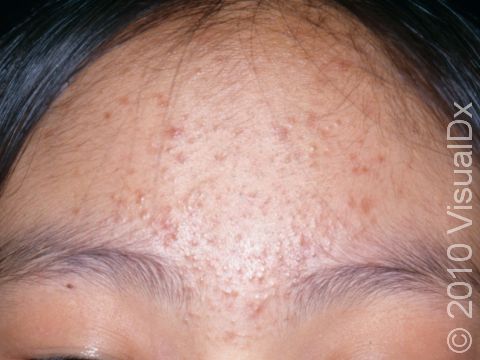
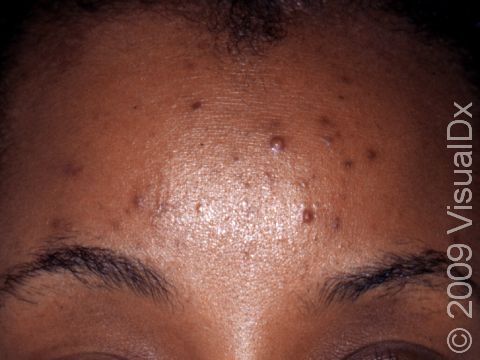
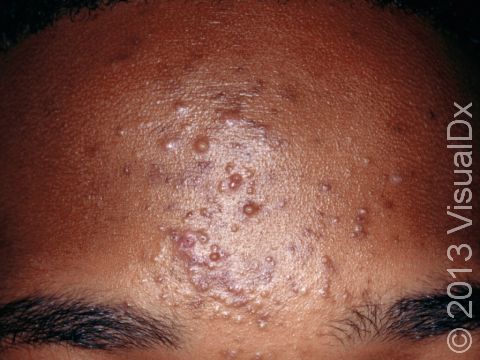
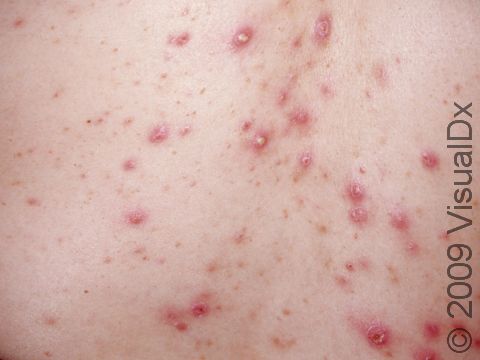
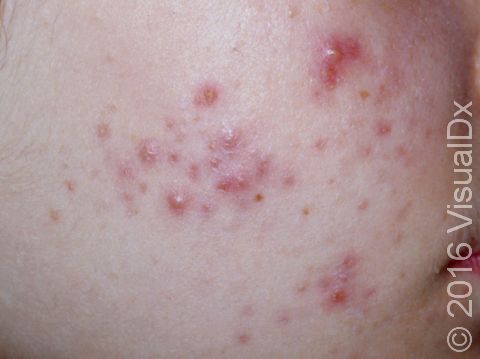
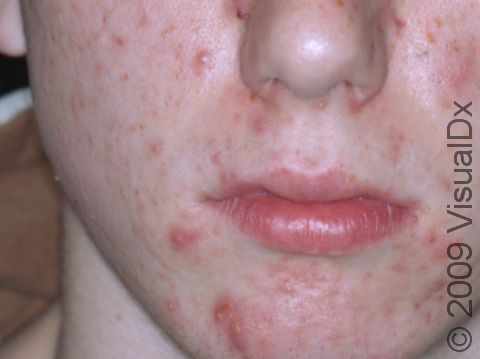
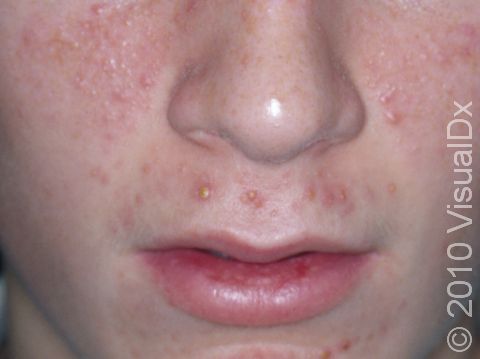
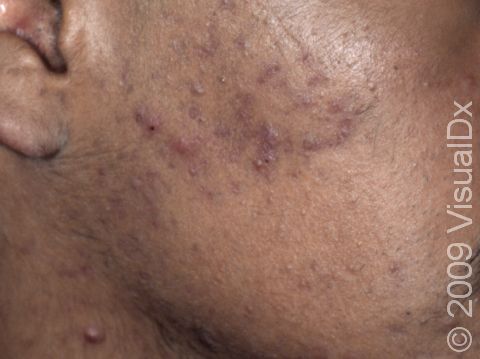
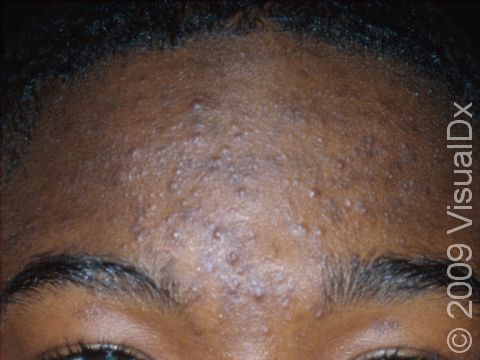
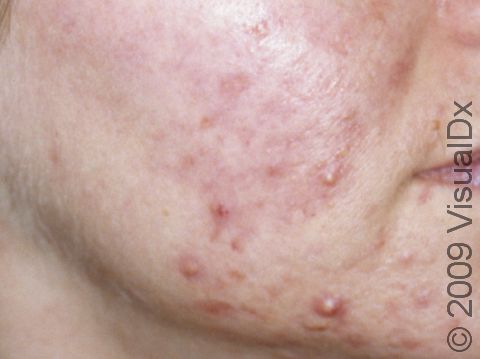
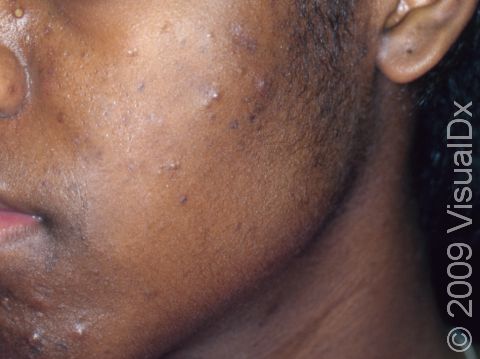
Acne results in a variety of skin lesions. The most common locations for acne lesions include the face, neck, chest, and back, where the most sebaceous glands are located. Along the jaw line is a common location for acne in adults. Acne lesions can be blackheads (open comedones), whiteheads (closed comedones), papules, pustules, and nodules / cysts. Papules are small, smooth, solid bumps that may be pink or red in lighter skin colors or darker red, maroon, or brown in darker skin colors. Pustules are pus-filled lesions, and nodules and cysts are larger and deeper than papules.
Mild acne consists of a few papules / pustules and sometimes comedones. Moderate acne has an increased number of these lesions. Severe acne has numerous comedones, papules, pustules, and may have painful nodules / cysts.
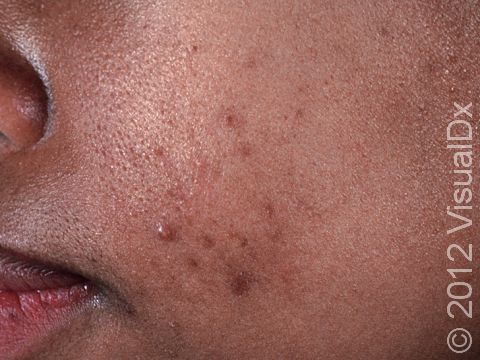
Acne can result in permanent scars, which can appear to be depressions in the skin or as hyperpigmentation, which appears as brown, flat marks where the acne lesions were. This skin color change may be more pronounced or last longer in darker skin colors.
Self-Care Guidelines
Gentle cleansing of acne-prone areas of the skin with gentle soaps or cleansers is an important aspect of general care in acne-prone skin. Avoid irritants such as rubbing and other alcohols, abrasive scrubs, and greasy products on the skin, including on the scalp (as this may spread to the face). Products labeled “water-based” or “noncomedogenic” will help reduce clogged pores. To avoid scarring, be sure to resist picking at the lesions. Sunscreens can minimize the appearance of hyperpigmentation, and noncomedogenic, tinted sunscreens are preferred.
Keep your hair, hands, and devices such as cell phones off your face.
Over-the-counter medications:
There are a variety of over-the-counter medications that may help. These are meant to be preventive therapies and should be applied in a thin layer to the entire area on a regular basis. If applied consistently, you may see small improvements quickly, but results are generally seen after a few months. Benzoyl peroxide (the most-effective over-the-counter medication) is available in a variety of formulations (such as washes, gels, and creams) and strengths. Benzoyl peroxide tends to dry the skin, though, so if you have dry skin, use a weaker-concentration product; for oily skin, consider higher strengths. Be aware that benzoyl peroxide can bleach your clothing and towels. Peeling agents (exfoliants) such as salicylic acid, sulfur, and alpha-hydroxy acids (such as glycolic acid) can help but will also cause some dryness of the skin.
Of note:
- Acne can have significant psychological effects. Talk to your doctor about any feelings of depression.
- Changes in diet have no proven effect on acne.
Treatments
Topical treatments for acne include one or more creams, washes, or gels, such as:
- Antibacterial agents such as clindamycin (Cleocin T), erythromycin (AkneMycin), sulfur (Liquimat, Sulpho-Lac), sodium sulfacetamide (Sulfacet R), dapsone (Aczone), minocycline (Amzeeq, Zilxi), and azelaic acid (Azelex, Finacea).
- Retinoids – vitamin A-derived products such as tretinoin (Retin-A), tazarotene (Avage, Tazorac), and adapalene (Differin).
- Clascoterone (Winlevi) – inhibits hormones that cause acne.
Oral treatments may include:
- Antibiotics such as tetracycline (Sumycin, Actisite), minocycline (Dynacin, Minocin), doxycycline (Vibramycin, Monodox), erythromycin, ampicillin (Ampi), clindamycin (Cleocin), trimethoprim-sulfamethoxazole (Bactrim), azithromycin (Zithromax), or cephalosporins.
- Oral contraceptives and spironolactone (Aldactone, CaroSpir) have been found to help regulate hormones.
- Isotretinoin (Amnesteem, Claravis), a strong drug with many side effects, for severe acne unresponsive to the above treatments.
Procedures:
- Steroid injections into any inflamed or stubborn nodules or cysts.
- Several types of laser treatments also help acne and are often used with other treatment methods; treatments are expensive, must be repeated for several months, and have variable results, though. Insurance may not cover laser therapy.
- Laser resurfacing, plastic surgery, and/or dermabrasion may help reduce the prominence of old acne scars.
- For hyperpigmentation, retinoids and benzoyl peroxide can speed up the process of lightening. Other products include topical hydroquinone, azelaic acid (10%-20%), glycolic acid, and kojic acid, and procedures such as microdermabrasion and light chemical peels can also be helpful.
Visit Urgency
If you have moderate or severe acne that has not improved enough with self-care, seek medical help.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on May 25th, 2023 at 11:36 am
Not sure what to look for?
Try our new Rash and Skin Condition Finder