Answering Your Questions About Psoriasis: A Guide
See more pictures of psoriasis
Psoriasis is one of the most common skin conditions treated by dermatologists, and it affects a significant proportion of the US population. Whether you know it or not, chances are you’ve already encountered several people in your life who have psoriasis. Let’s learn a bit more about psoriasis by going over 10 common questions you might have.
1. What is psoriasis?
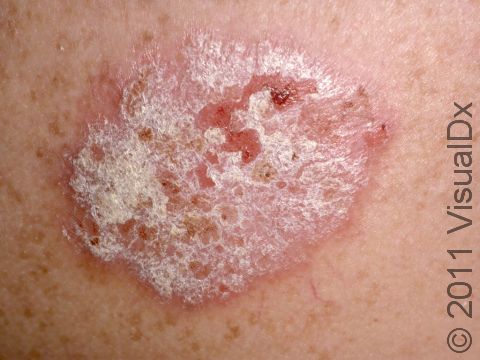
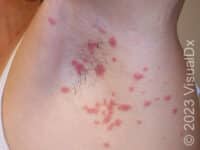
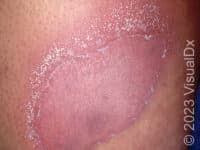
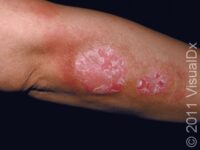
Psoriasis is a chronic skin condition that results in plaques (raised areas of skin that are larger than a thumbnail) with characteristic white overlying scale. The plaques are commonly located on the trunk, knees, elbows, belly button, genitals, and scalp. Psoriasis plaques are typically pink or salmon colored, with sharp, well-defined borders. The picture below shows an example of a psoriatic plaque that demonstrates the classic features described. While this is the most common clinical presentation, known as plaque psoriasis, psoriasis has several other variants and may present in other, nontraditional ways.
2. How common is psoriasis?
Psoriasis is one of the most common skin conditions in the United States, affecting approximately 3% of the US population. This means that the total number of individuals living with psoriasis in the US is more than 7.5 million, which is about the entire population of New Jersey. Due to its high prevalence and chronic nature, the total cost of psoriasis in the US is estimated to be around $23 billion each year, including the cost of treatments as well as indirect costs, such as time lost at work by individuals affected by psoriasis.
3. What causes psoriasis?
The exact cause of psoriasis is complex and not yet fully understood. However, psoriasis research has identified multiple factors that may contribute to this condition. The most important factor is the immune system. Many experts consider psoriasis an autoimmune disease, meaning that the immune system is overactive or increased and results in direct damage to the skin, joints, and other organs in the body. Genetic susceptibility also contributes to the onset of psoriasis as it tends to occur in certain families and is associated with more than 80 genes that have a strong association with increased psoriasis risk. Other factors may trigger psoriasis or cause worsening of symptoms, such as stress, pregnancy, certain medications, bacterial infections such as strep, skin injury, or use of tobacco and alcohol.
4. Is psoriasis dangerous or contagious?
Psoriasis isn’t contagious and is very rarely dangerous. The majority of psoriasis patients, especially those who are adequately treated, will go on to live normal, happy lives. Certain rare forms of psoriasis, such as erythrodermic or generalized pustular psoriasis (GPP), can potentially be life-threatening, though, and can pose an immediate health risk if left untreated. Importantly, research in the last decade has shown that having psoriasis also increases your risk for other health conditions, such as psoriatic arthritis (autoimmune attack of the joints, tendons, or ligaments potentially leading to permanent bone loss), cardiovascular disease, stroke, high blood pressure, obesity, diabetes, sleep disorders, psychosocial disorders such as depression or anxiety, kidney disease, and cancer. This means choosing not to treat your underlying psoriasis has its own health risks.
5. Areas of my skin recurrently get red and scaly, so do I have psoriasis?
Not necessarily. Psoriasis is one of many skin conditions that can result in red, scaly skin. For this reason, it’s important to be examined by a dermatologist or rheumatologist if you have a chronic rash or joint symptoms, respectively. Many people who go to a dermatologist for evaluation of their presumed “psoriasis” are often diagnosed with another skin condition that mimics psoriasis. These conditions include atopic dermatitis (eczema), seborrheic dermatitis (dandruff), intertrigo, fungal infections of the skin, allergic or irritation reactions in the skin, other autoimmune conditions such as lupus, and adverse drug reactions, among others. All these similar conditions can look identical to psoriasis and often require a well-trained medical professional to help determine the exact diagnosis.
6. My friend told me that my psoriasis is most likely caused by my stress or gluten in my diet. Is this true?
Since psoriasis is rarely present at birth and develops later in life (most commonly in young adulthood or around retirement age), it is understandable for people to wonder if there is an environmental cause for their condition. While increased stress or an unhealthy diet may cause worsening of your psoriasis, it is not the primary reason for your condition. As mentioned previously, psoriasis is primarily driven by your overactive immune system and inherited genes, neither of which are within your direct control. It’s important for individuals with psoriasis to understand that they are not responsible for causing their psoriasis, although lifestyle modifications or changes may be helpful in reducing the severity of their condition or symptoms. For example, people with psoriasis often notice considerable improvement in their psoriasis with increased exercise, a healthier diet (eg, low sugar, low carb, or a Mediterranean diet), and decreased levels of stress. To date; however, there is no evidence that eliminating stress and/or avoiding specific dietary components such as dairy or gluten will result in complete resolution of psoriasis with no other medical treatments.
7. How do I know which treatment is best for my psoriasis?
The treatment of psoriasis is very complex and can be difficult to navigate on your own as a patient. This is because many highly effective medical treatments are available and often require prior approval by your insurance provider. Additionally, a specific treatment regimen used in one patient with no other medical issues may be inappropriate or even harmful in another patient with several other medical conditions (eg, cancer or pregnancy). Finally, it is imperative for your dermatologist or rheumatologist to assess several factors of your psoriasis before selecting a specific treatment, such as which body sites are affected, the extent of your psoriasis (eg, localized or widespread), your symptoms, and any ways in which your disease is interfering with your personal or work life. Talking with your medical professional about the advantages and disadvantages of the various treatments will help you choose the right psoriasis treatment for you.
8. What are some of the most common treatments used today for psoriasis?
Since the primary driver of psoriasis is an overactive immune system, all effective psoriasis treatments work by helping normalize the immune system and counteracting the inflammatory response causing your skin changes, joint pain, and other symptoms. Topical steroids are one of the mainstays of treatment for mild or localized forms of psoriasis as they can help reduce inflammation and stop the progression and formation of psoriasis plaques. Unlike oral steroids, topical steroids are safe when used properly and do not have systemic effects on the body. Salicylic acid, T/Gel shampoo, and other medications designed to remove skin flakes and scales (known as keratolytics) are another treatment option that can be used to remove the scale and help reduce the thickness of psoriatic plaques. Other commonly used topical agents include vitamin D derivatives, retinoids, and tar treatments. Ultraviolet light from natural sun exposure or in-office UV light treatments (called phototherapy) can improve psoriasis through its anti-inflammatory effects, which can be useful for more widespread psoriasis.
More severe cases of widespread psoriasis, psoriatic arthritis, or disease that affects special skin sites, such as the face, scalp, genitals, or palms and soles, may require the use of oral or injectable medications. Traditional oral medications, such as methotrexate or cyclosporine, are broad-acting medications that prevent the detrimental effects of too much inflammation. However, these medications are also associated with several significant side effects and should be used with caution and under the direction of a dermatologist or rheumatologist familiar with them. Oral steroids are not an appropriate treatment for psoriasis and should be avoided as they can result in severe worsening of psoriasis once the oral steroid is stopped. The good news is newer nonsteroid oral medications have been developed for the treatment of psoriasis that work well in most individuals with relatively few side effects. And there is more good news: an even newer class of medication, called biologics, are particularly promising. Biologic medications contain proteins that are injected into the skin and work like snipers in the body that target the inflammatory signals causing psoriasis without impacting other aspects of normal health. Biologic medications for psoriasis are extremely effective and often result in complete resolution of skin disease with few side effects.
9. Are there treatments that can put psoriasis into long-term remission?
Laboratory and clinical research have made tremendous advances in our understanding of psoriasis and its response to specific immune treatments. The field has remained focused on treatments that could potentially “cure” psoriasis – or at least put the condition into long-term remission. Such treatments, unfortunately, do not yet exist and are still being studied. Nevertheless, clinical trials have shown that multiple FDA-approved biologic medications achieve near-complete clearance of the skin in psoriasis patients with as few as 4 injections into the skin per year. These novel biologic treatments result in such dramatic improvements in psoriasis that patients are often able to experience life again without any visible signs or symptoms of their disease!
10. Where can I get additional information about my psoriasis or find a support network with others who also live with psoriasis?
There are several organizations and foundations that work hard to offer quality medical information and provide social support to patients living with psoriasis. These organizations include the National Psoriasis Foundation (NPF), the American Academy of Dermatology (AAD), and the International Psoriasis Council (IPC). The NPF also offers psoriasis patients the opportunity to interact directly with NPF staff and volunteers to help them navigate the complexities of the health care system and the many psoriasis treatments. There are countless psoriasis forums and support groups online and on social media platforms, but note that the medical information shared on certain online platforms may be incorrect or not supported by good clinical evidence.
Sources/Further Reading
Last modified on August 31st, 2023 at 3:58 pm