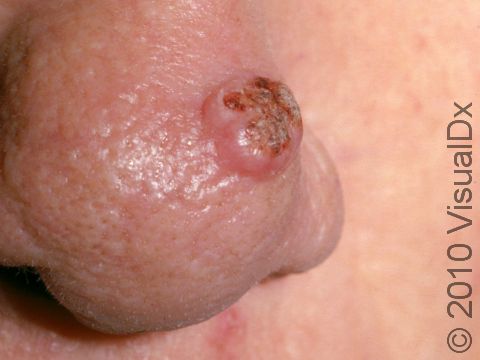
Keratoacanthoma
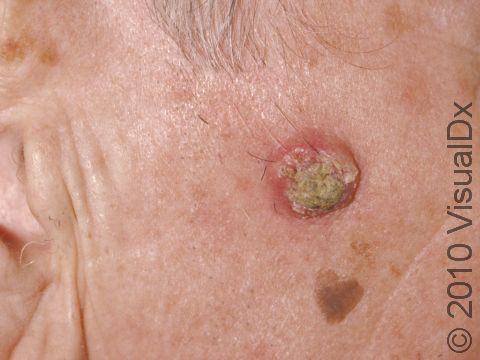
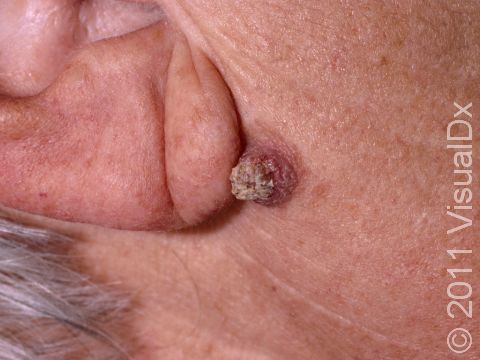
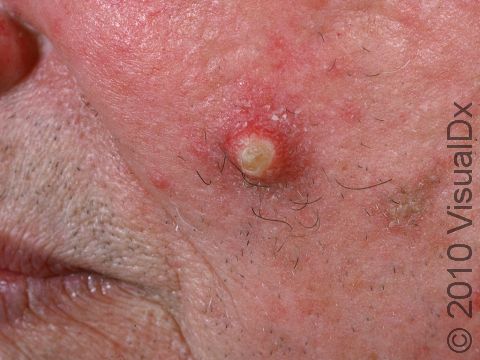
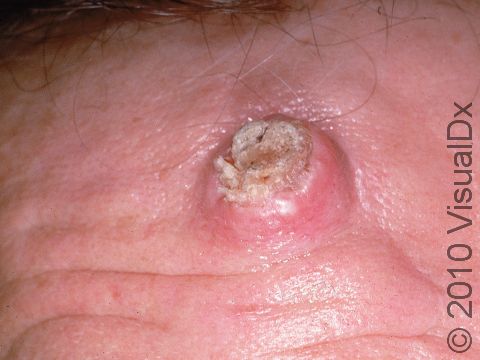
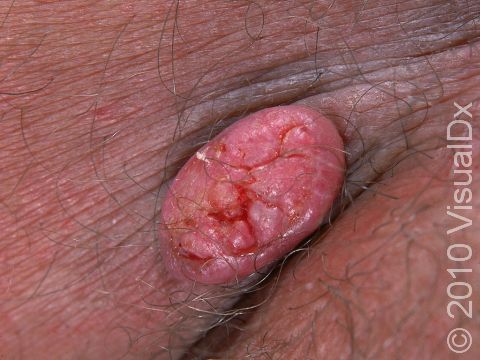
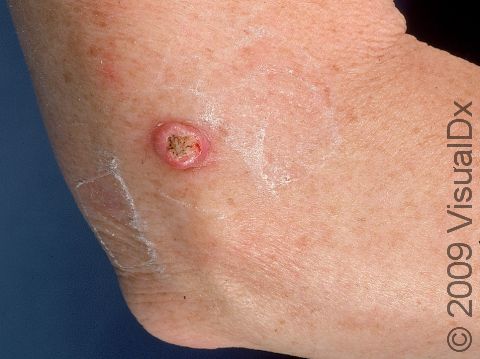
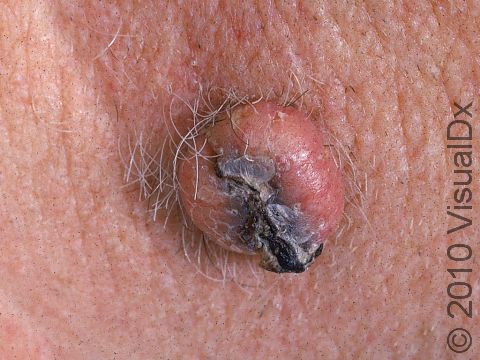
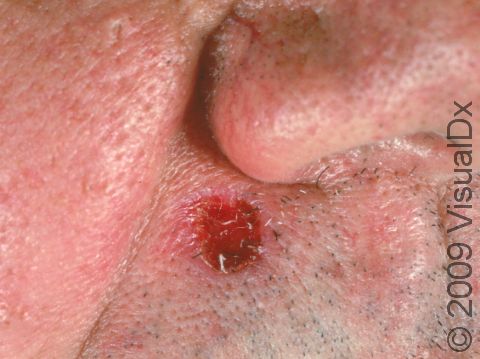
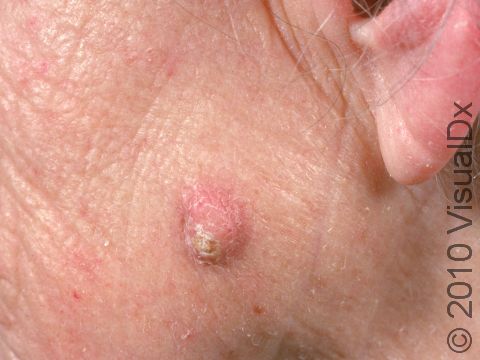
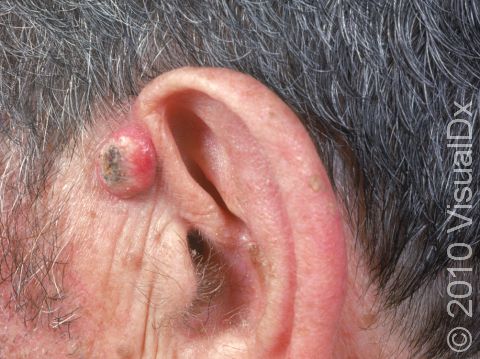
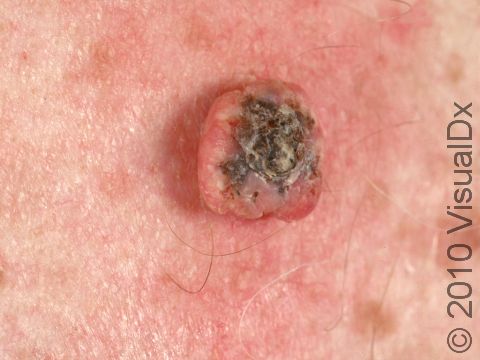
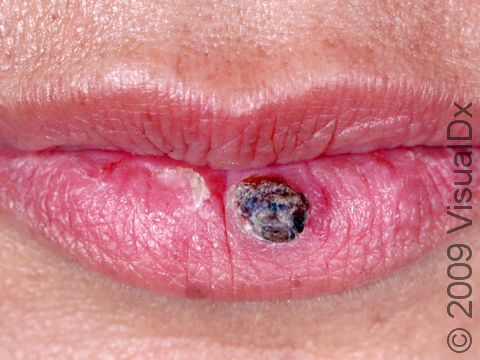
A keratoacanthoma is a rapidly growing skin cancer that usually appears as a volcano-like nodule (a solid bump that is firm to the touch) on the sun-exposed skin of middle-aged or older individuals. They are thought to be a type of squamous cell carcinoma. Most keratoacanthomas arise quickly (within a few weeks to a month) and then may self-resolve within 6 months, leaving just a scar. However, they may persist and continue to grow, and sometimes eventually spread to lymph nodes.
Who's At Risk?
Keratoacanthomas are most commonly seen in older adults with lighter skin colors who have a history of sun exposure.
Risk factors for the development of keratoacanthoma include:
- Age over 50 years.
- Lighter skin colors, light hair, or light eyes.
- Male sex.
- Chronic exposure to sunlight or other ultraviolet (UV) light.
- Exposure to certain chemicals, such as tar.
- Exposure to radiation, such as x-ray treatment for internal cancers.
- Long-term immunosuppression, such as in organ transplant recipients.
- Long-term presence of scars, such as from a gasoline burn.
- Chronic ulcers.
- Presence of particular strains of the virus that causes warts (human papillomavirus).
- Previous skin cancer.
Signs & Symptoms
A keratoacanthoma appears and grows rapidly over the course of 2-6 weeks. Starting as a small, pimple-like lesion, a keratoacanthoma typically develops into a dome-shaped, skin-colored nodule with a central depression filled with keratin (the major protein found in hair, skin, and nails). Keratoacanthomas usually range in size from 1-2 cm.
The most common locations for keratoacanthoma include the:
- Center of the face.
- Backs of the hands.
- Arms.
- Ears.
- Scalp.
- Lower legs, especially in women.
In rare cases, multiple keratoacanthomas may develop. Most keratoacanthomas are painless, but some may be itchy.
Self-Care Guidelines
There are no effective self-care treatments for keratoacanthoma. Preventing sun damage is crucial to avoiding the development of keratoacanthoma:
- Avoid UV light exposure from natural sunlight and from artificial tanning devices.
- Wear broad-spectrum sunscreens (blocking both UVA and UVB) with sun protection factor (SPF) 30 or higher, reapplying frequently.
- Wear wide-brimmed hats and long-sleeved shirts.
- Stay out of the sun in the middle of the day (between 10:00 AM and 3:00 PM).
Treatments
If your medical professional suspects a keratoacanthoma, they will first want to establish the correct diagnosis by performing a biopsy.
Once the diagnosis of keratoacanthoma is established, the treatment options usually include:
- Removal (excision), in which a scalpel is used to cut away the keratoacanthoma and then place stitches to bring the wound edges together.
- Mohs micrographic surgery, in which tiny slivers of skin are removed until there are no more cancer cells. This technique is particularly useful for keratoacanthomas located on the nose, ears, lips, and hands.
- Electrodesiccation and curettage, also known as “scrape and burn.” After numbing the lesion, the medical professional uses a sharp instrument called a curette to scrape away the skin cancer cells, followed by an electric needle to burn (cauterize) the tissue. The electrodesiccation helps kill the cancer cells and stop bleeding at the site.
- Radiation treatment, where x-ray therapy is often useful for patients who may have difficulty with a surgical procedure due to other health issues.
Very rarely, keratoacanthomas are treated with medicine injected directly into the skin lesion (intralesional chemotherapy). In patients with more than one keratoacanthoma, the medical professional may suggest taking oral medication (ie, isotretinoin) to reduce their size and number.
Once the skin cancer has been removed, frequent follow-up appointments with a dermatologist or medical professional trained to examine the skin are essential to ensure that the keratoacanthoma has not returned and that no new skin cancer has developed elsewhere on your body. In addition, good sun protection habits (as noted in the Self-Care section) are vital to preventing further damage from UV light.
Visit Urgency
If you develop a new growth on sun-exposed skin or a lesion that bleeds easily or does not seem to be healing, make an appointment with a medical professional such as a dermatologist. You should also seek care if an existing lesion changes size, shape, color, or texture, or if it starts to itch, bleed, or become sore to the touch.
Be sure to mention when you first noticed the lesion and what symptoms, if any, it has. Young adults should ask adult family members if they have ever had skin cancer and relay this information to the medical professional.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 17th, 2024 at 3:44 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder