Lymphogranuloma Venereum (LGV)
Lymphogranuloma venereum is an uncommon sexually transmitted infection (STI) caused by infection with the bacteria Chlamydia trachomatis. It is spread through having unprotected vaginal, oral, or anal sex. Lymphogranuloma venereum causes painful and swollen lymph nodes, which can then break down into large ulcers (open sores). The disease goes through 3 distinct stages as it develops. The first 2 stages of lymphogranuloma venereum may be minor, and you might not even be aware of any symptoms until you reach stage 3, called the genitoanorectal syndrome.
Who's At Risk?
Lymphogranuloma venereum has been found in people all over the world, but it is more commonly seen in tropical and subtropical countries. It is uncommon in the United States and Europe, but in recent years, more outbreaks have occurred in both areas, most often in White men who have sex with other men and who are infected with HIV.
Lymphogranuloma venereum is most common in those aged 15-40 years. Men are often diagnosed in the earlier stages (likely because it is more visible in men) than women, who are often diagnosed in later stages, often with complications. Anyone who has sex without condoms is at risk of becoming infected with lymphogranuloma venereum.
Signs & Symptoms
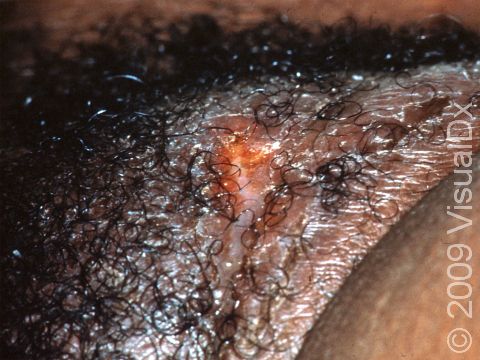
In the first stage of lymphogranuloma venereum, after a 3-30 day period, a small, painless papule (solid bump) or pustule (pus-filled bump) forms on the penis, scrotum, vulva, or in the vagina that may open and form an ulcer. If the infection is in the anus, there may be blood or mucus in the stool. This lesion often has no symptoms and heals without scarring within about a week.
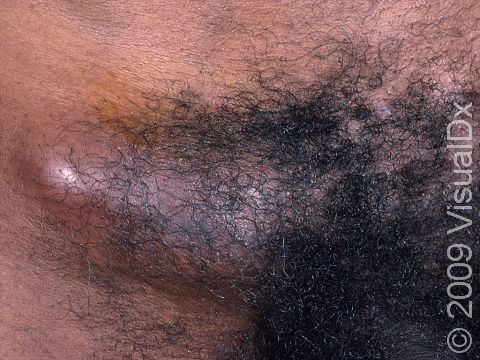
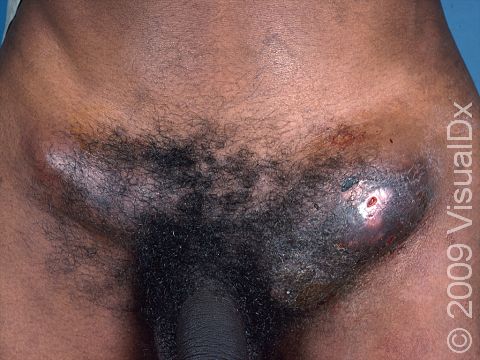
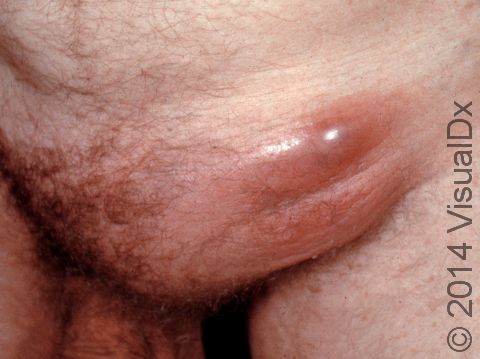
The second stage begins 2-6 weeks after the first lesion appeared and consists of painful swelling of the groin or other lymph nodes. Individuals may develop fever, chills, and fatigue. The painful, swollen lymph nodes become enlarged and may open and drain, or they may become hard and then slowly heal on their own. Women may not have any visible lymph nodes and have only mild back or belly pain.
In the third stage, those who have been infected in the anus have rectal infection (proctocolitis), which can cause pain with passing stool, deep boils (abscesses), and scarring. When the infection is in the genital tract, there may be enormous swelling of the genitals as well as draining from the areas of infected skin.
Self-Care Guidelines
Do not attempt self-care if you suspect you might have lymphogranuloma venereum or if you have any sore or ulcer on the genital or rectal area. Avoid sexual intercourse, notify all sexual contacts, and see your medical professional.
To prevent lymphogranuloma venereum infection, avoid sexual activity, or maintain a mutually monogamous long-term relationship with someone who is not infected and use latex condoms consistently and correctly when engaging in sexual activity.
Treatments
Your medical professional may recommend blood and fluid culture tests as well as testing for other STIs, such as gonorrhea, syphilis, HIV, hepatitis, and chlamydia.
Antibiotics can treat the infection and prevent further damage to the skin, but there may be some resultant scarring. Your medical professional may drain the infected areas to prevent ulcers from forming.
Visit Urgency
If you suspect that you or a partner may have lymphogranuloma venereum, or if you have a sore or discharge from the genital or rectal area, avoid sexual intercourse, notify all sexual contacts, and see your medical professional.
Anyone who has had sexual contact with a person with lymphogranuloma venereum within the 60 days before the onset of symptoms should be examined and tested for lymphogranuloma venereum.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 14th, 2024 at 3:29 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder