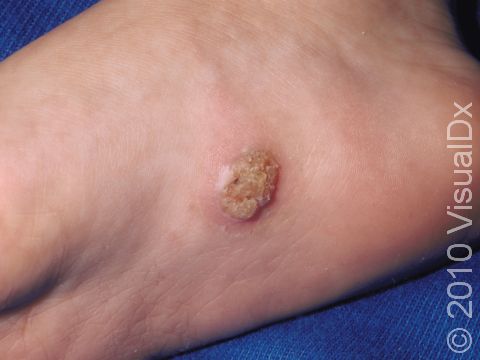
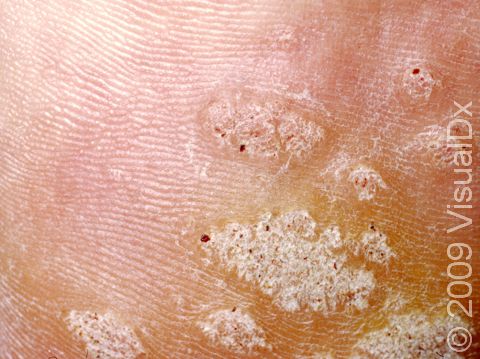
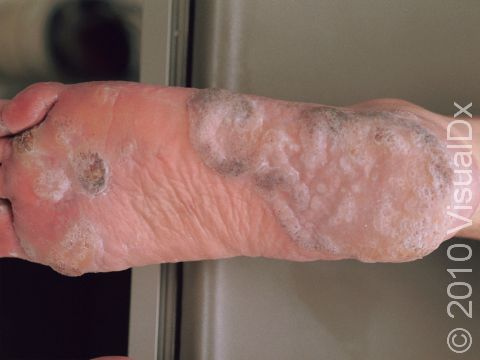
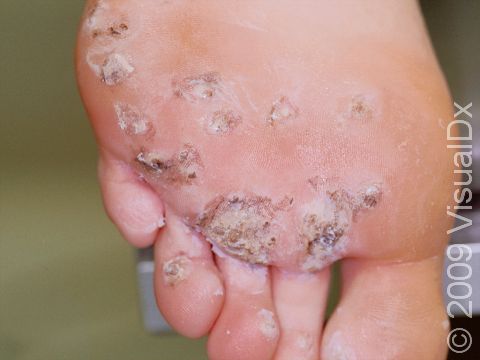
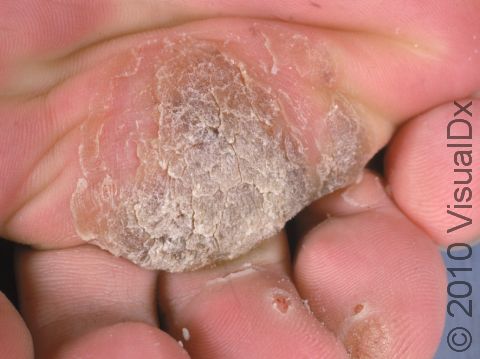
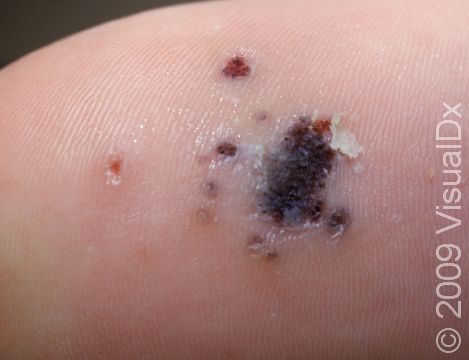
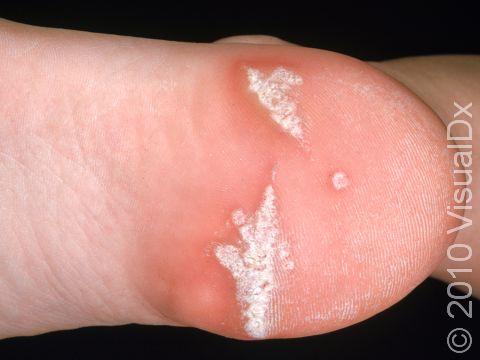
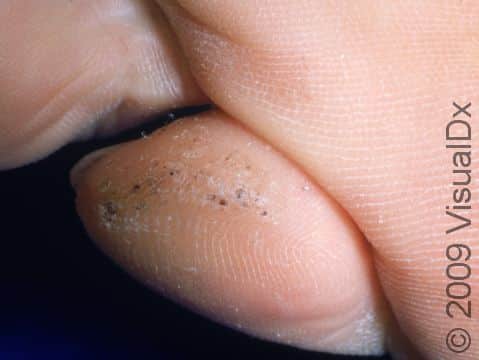
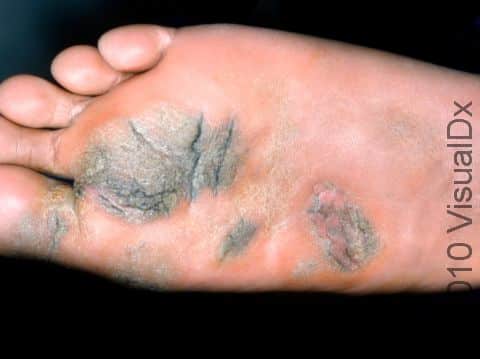
Plantar Wart
Warts are growths of the skin and mucous membranes (the mouth or genitals) that are caused by a virus known as the human papillomavirus (HPV). The virus causes thickening of the top skin layer. Plantar warts occur on the sole of the foot. They can look and feel like a callus. Plantar warts can be small, or they can grow to cover most of the sole of the foot. They can be painless or may be tender. They may go away on their own, sometimes taking a few months or up to a couple years to resolve.
Warts are usually acquired from person-to-person contact. The virus is not highly contagious but can cause an infection by entering through a small break in the skin. In the same way, warts can be spread to other places on your own body (self-inoculation). The virus can sometimes be transferred by touching an object used by an infected person.
Who's At Risk?
Warts can affect people of any age, but they are most common in those aged 12-16 years. It is estimated that 20% of schoolchildren and about 10% of the general population have warts. People with HIV or organ transplants or those who are on chemotherapy have a higher incidence of warts due to their weakened immune system.
Signs & Symptoms
The most common locations for plantar warts include the:
- Soles of the feet, especially the weight-bearing areas (eg, the heels and balls of the feet).
- Undersides of the toes.
Plantar warts may occur singly or in clusters. They appear as thick, rough, callus-like thickenings on the soles of the feet. In addition, plantar warts often have what appear as multiple small black “dots” at the surface, which are actually tiny blood vessels.
Plantar warts can be painful when pressure is applied, such as from walking.
Self-Care Guidelines
Because warts can resolve on their own, it is not necessary to treat all warts. Additionally, treating warts may not always destroy them, nor will it necessarily keep other warts from appearing. Treatment can be painful, cause scars, and may need to be repeated, so treatment should only be done in cases where the warts are highly bothersome or interfere with daily life.
- Duct tape applied daily to the affected area can help treat plantar warts. The tape should be very sticky and kept on for a few days at a time. Between changes of duct tape, the wart should be soaked in warm water, and any loose skin should be removed every few days with a mild abrasive, like a pumice stone or emery board.
- Over-the-counter wart removers contain salicylic acid and work by dissolving away the layer of skin infected with the virus. This treatment needs to be used daily and can sometimes be irritating to skin around it; 40% salicylic acid self-stick pads appear to be one of the most effective types. Keep each pad on for 2-3 days. Remove the pad and tape, and scrub away the top layer of dead skin, now white-colored, with an emery board or pumice stone. Reapply a new 40% salicylic acid pad. Keep removing dead skin and reapplying every few days until the wart is gone. Many plantar warts will respond in 1-2 months.
- Over-the-counter freezing medications are available but have not been found to be very effective.
- Household members should avoid sharing personal items such as towels.
Treatments
Once you have been diagnosed with a plantar wart, your medical professional may try one or more of the following treatments:
- Freezing with liquid nitrogen (cryosurgery)
- Burning with an electric needle (electrocautery)
- Using a laser to disrupt the blood supply of the warts
- Application of podophyllin, tretinoin, or salicylic acid
- Injection with Candida antigen, which causes an immune reaction that may destroy the wart
- Injection of a chemotherapy drug (bleomycin) into the wart
Plantar warts can be very stubborn, and effective treatment may take many months.
Visit Urgency
Make an appointment with a medical professional if you have:
- Painful or bleeding warts.
- Rapidly spreading or multiplying warts.
- Warts that interfere with daily life and are not responsive to self-care.
People with diabetes or a circulatory disorder should have their warts treated by a physician.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 26th, 2024 at 12:02 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder