Stasis Dermatitis
Dermatitis is a term used to describe irritation of the skin with scaling, rough or dry skin, redness, itching, and sometimes oozing, crusting, and erosions. Stasis is a term used to describe leg swelling seen in conditions of poor circulation and fluid buildup.
Stasis dermatitis is skin irritation and breakdown due to the fluid accumulating under the skin.
Stasis dermatitis can be due to venous insufficiency (vein valve malfunction), heart failure, and other conditions that cause swelling, usually in the legs.
Who's At Risk?
Stasis dermatitis most often occurs in adults older than 50. The risk of developing stasis dermatitis increases with age. Women are slightly more likely to be affected, perhaps due to the effect of pregnancy on the leg vein system.
When seen in younger people, stasis dermatitis is usually caused by vein valve malfunction from surgery, trauma, a history of deep vein blood clots, or repeated infections.
Signs & Symptoms
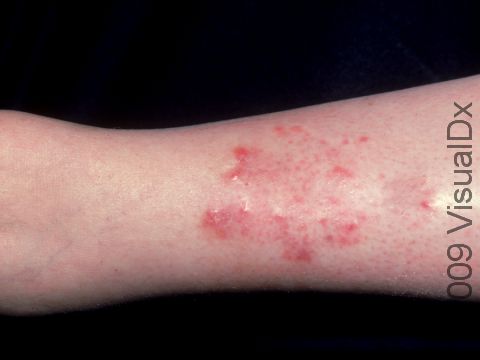
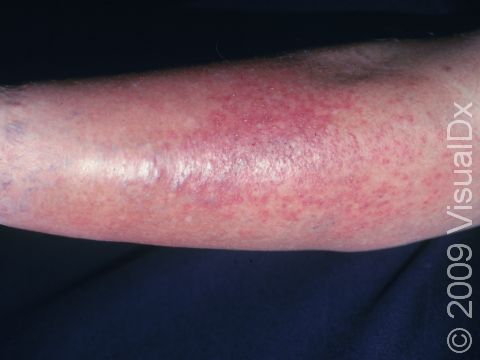
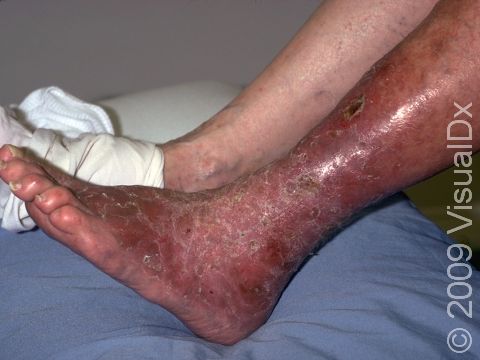
Itching and red, dry, scaly papules (small, solid bumps) or plaques (raised or bumpy areas larger than a thumbnail) are usually the first signs of stasis dermatitis. The inside ankle area is often first affected, gradually involving the lower leg up to the knee. The skin may also appear shiny or have reddish-brown patches. In darker skin colors, the redness may be hard to see or may appear more purple.
Swelling (edema) is usually present, but in chronic cases of stasis dermatitis, there is gradual tightening and scarring of the skin, leading to hard and sometimes tender areas.
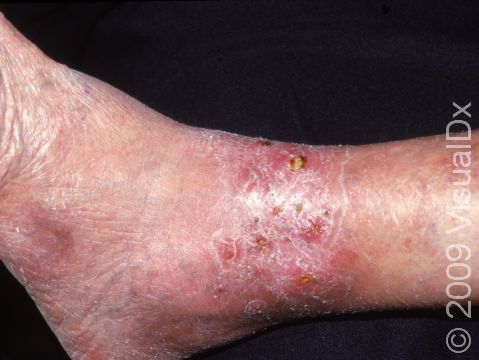
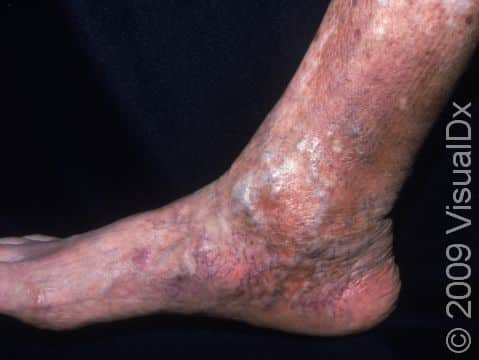
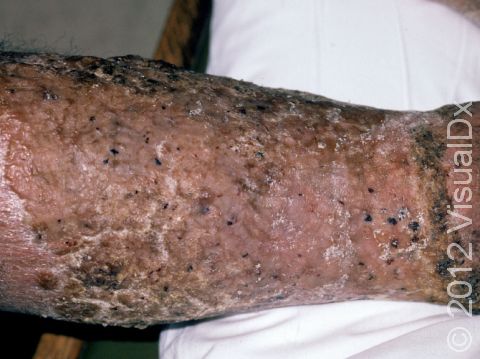
In severe cases of stasis dermatitis, the skin breaks down with oozing, crusted areas, and ulceration (a wound or sore with missing skin). White, shiny scars are often left after healing.
In longstanding cases, there may be significant thickening and darkening of the skin from rubbing.
Self-Care Guidelines
The most important step is to correct the underlying problem causing the fluid buildup. It is also important to understand that the condition is usually a chronic one requiring ongoing care for the rest of one’s life.
If the stasis dermatitis is mild and clearly related to leg swelling, which is minimal upon arising in the morning but worse after a day of standing, simple measures can assist the veins and reduce the chance of progression of the disease, requiring medical care.
These steps include:
- Elastic support hose (worn to at least knee height) should be put on in the morning upon arising. Many nonprescription and attractive styles are available. Although they are initially tight, discomfort is less as the swelling is controlled.
- Raising the legs above the level of the heart when sitting reduces fluid buildup.
- Moving / exercising as tolerated. Muscle movement helps circulation.
- Applying 1% hydrocortisone cream (available over the counter) to the red, itchy areas twice daily.
- Practicing a proper skin-care routine, which includes using only mild soaps or cleansers and applying a moisturizer on the legs (such as petroleum jelly [eg, Vaseline]) after each bath or shower.
- Avoiding the use of other creams or topical antibiotics, as allergic reactions are common.
- Avoiding trauma to the area as much as possible.
Treatments
Your medical professional will do an examination to determine the cause of the swelling; vein studies may be suggested and, rarely, a culture or skin biopsy may be done. Compression stockings (specially designed stockings that apply pressure to the leg to prevent fluid from pooling) may be recommended.
Stronger corticosteroid creams or ointments may be used for short periods (not prolonged periods, however, due to the possible thinning of the skin from chronic use). Infection may be treated with oral or intravenous antibiotics. Oral medications may be used to control heart failure or reduce the presence of fluid.
Visit Urgency
Seek medical care if your legs are swollen. Also seek help if the itchy areas do not improve with self-care.
See a medical professional if there are signs of infection, including pain, fever, increased swelling and redness, or open areas accompanied by pus.
Ulcers or sores require medical attention.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 17th, 2024 at 12:34 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder