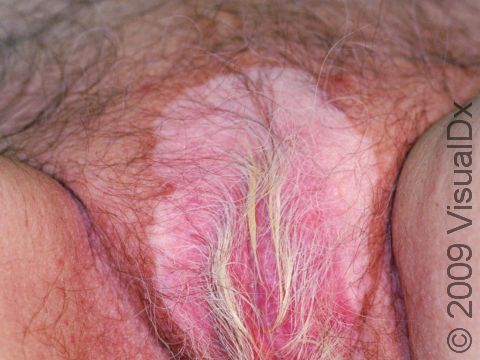
Vitiligo
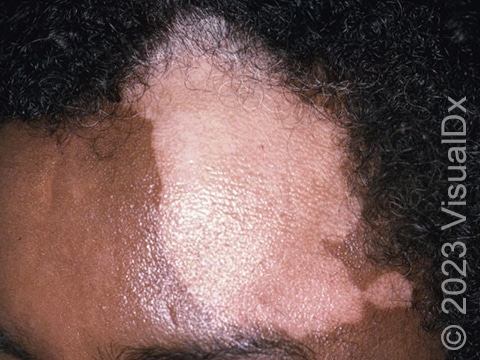
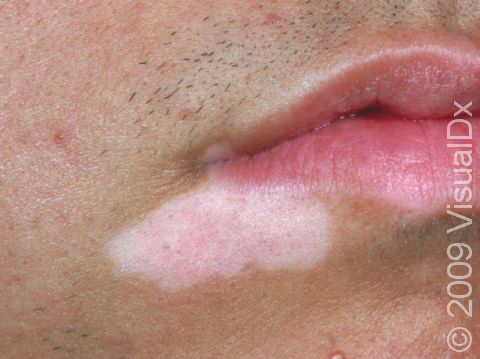
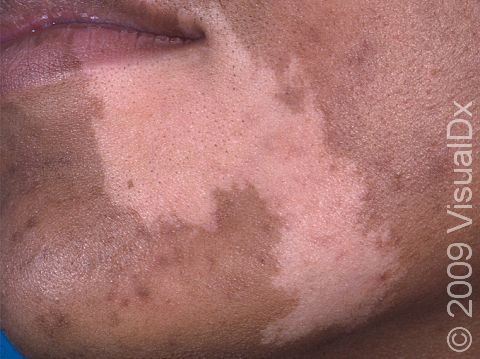
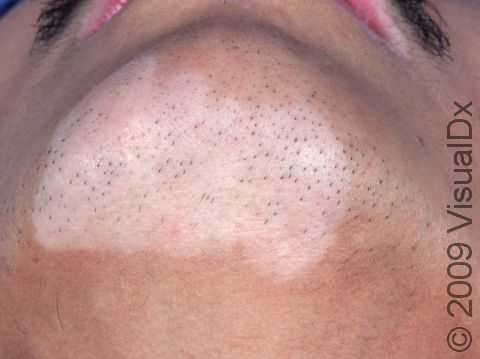
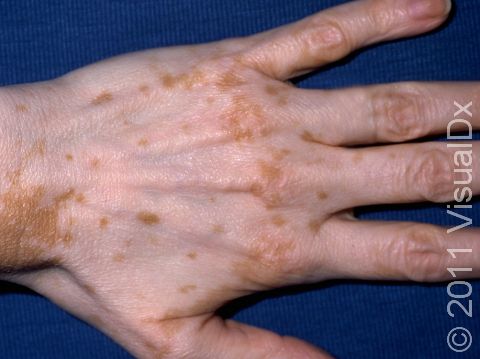
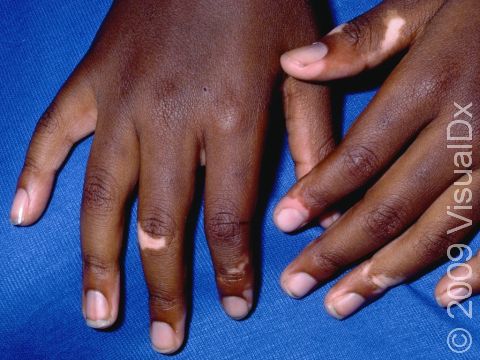
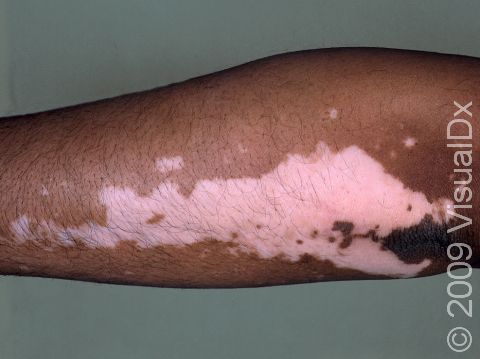
Vitiligo is a condition caused by the immune system turning against itself (an autoimmune disease). Immune cells of the body attack the color-producing (pigment-producing) cells in the skin, which leads to the formation of white (depigmented) patches that are often much larger than a thumbnail. In darker skin colors, the contrast between the normal pigmented skin and depigmented areas is greater than in lighter skin colors.
It may be seen with other autoimmune diseases, such as thyroid disease, alopecia areata, diabetes mellitus, Addison disease, and myasthenia gravis.
The way that vitiligo progresses varies greatly; it may remain in the area where it started (localized) or it may become more widespread.
Who's At Risk?
Vitiligo may start at any age but usually begins between the ages of 2 and 40. All races / ethnicities may be affected. Despite a common belief, vitiligo is not more common in Black individuals; however, the contrast between affected and normal skin is more obvious and potentially more cosmetically bothersome in individuals with darker skin.
Signs & Symptoms
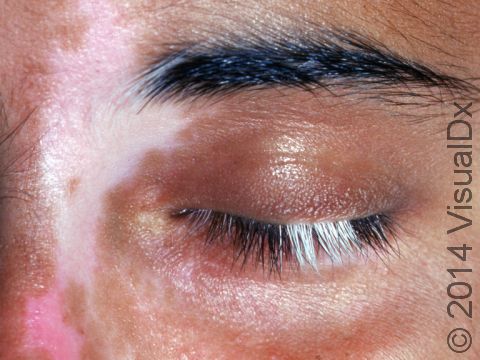
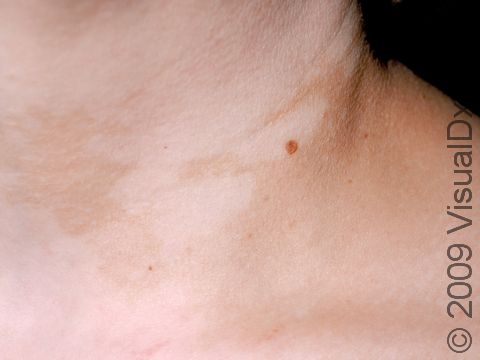
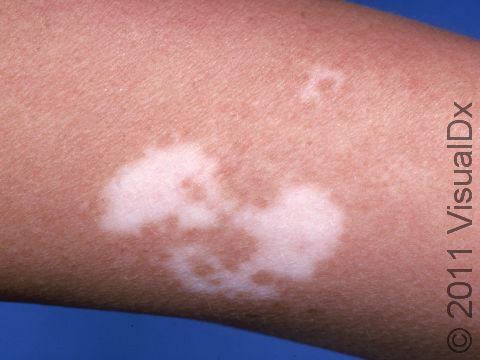
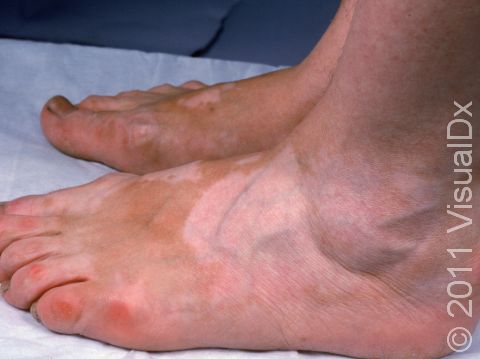
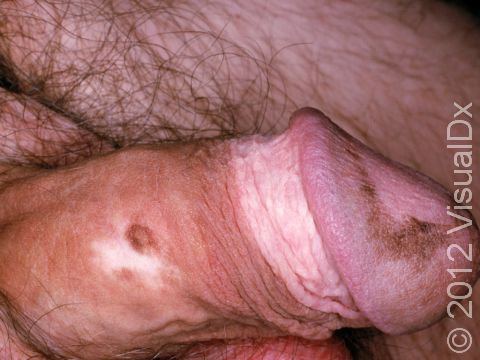
Vitiligo may affect areas prone to chronic minor injury, such as the fingers, knuckles, and elbows. It may also affect the face, upper chest, hands, underarms, and groin. It may be widespread, affecting both sides of the body (generalized); it may affect only one side of the body (segmental); or it may affect only one localized area (focal).
Sharply defined white patches are seen. If the affected area contains hair, the hair may turn white.
Sometimes halo nevi can be seen, which is a mole surrounded by a circular white patch, resembling a halo.
Self-Care Guidelines
It is important to protect your child’s skin from the sun, particularly the affected areas:
- Avoid exposure to midday sun (10 AM to 3 PM).
- Wear a broad-spectrum, high sun protection factor (SPF higher than 30) sunscreen.
- Wear protective clothing and hats.
Dermablend or Covermark cosmetic cover-up makeups can hide the white patches.
Treatments
Your medical professional may try any of the following:
- Topical steroid creams or ointments to help restore skin color. Use these with caution because of the risk of tissue damage (atrophy) with prolonged use, particularly on the face and skin fold areas.
- Topical nonsteroid medications, such as ruxolitinib (Opzelura) cream, tacrolimus (Protopic) ointment, and pimecrolimus (Elidel) cream.
- Ultraviolet (UV) light therapy or laser therapy.
- Superficial skin grafts, especially in hard-to-treat (recalcitrant) locations, such as over joints.
- For very large or widespread lesions, topical chemicals can remove color from (depigment) the normal skin.
Visit Urgency
It is not necessary to treat vitiligo, but seek medical evaluation if it becomes bothersome or if it is progressing.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 13th, 2024 at 12:12 pm
Related Skin Conditions


Not sure what to look for?
Try our new Rash and Skin Condition Finder