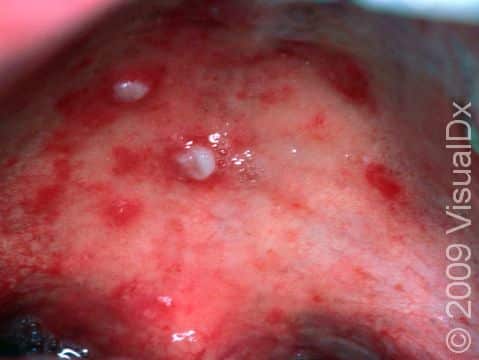
Hand, Foot, and Mouth Disease
Hand, foot, and mouth disease is a common illness caused by viruses of the enterovirus group, particularly coxsackieviruses. The disease is highly contagious and often spreads from child to child or from child to adult. Spread of the disease occurs by direct contact with nasal and/or oral secretions and stool contact. The incubation period from infection to symptoms is about 3-6 days. Outbreaks of hand, foot, and mouth disease usually occur from June to October.
Hand, foot, and mouth disease is usually not serious. Complications can occur, though, and they may include pneumonia, inflammation of the heart or brain, or miscarriage in pregnant individuals who become infected.
Hand, foot, and mouth disease is not related to foot-and-mouth disease seen in animals.
Who's At Risk?
Hand, foot, and mouth disease most often occurs in infants and children younger than 10 years, but teens and adults can also get it. It is commonly transmitted in day cares, schools, and summer camps.
Signs & Symptoms
Hand, foot, and mouth disease begins with a fever, sore throat, sore mouth, cough, headache, fatigue, loss of appetite or diarrhea / vomiting, and, occasionally, joint pain. After 1-2 days, a rash appears.
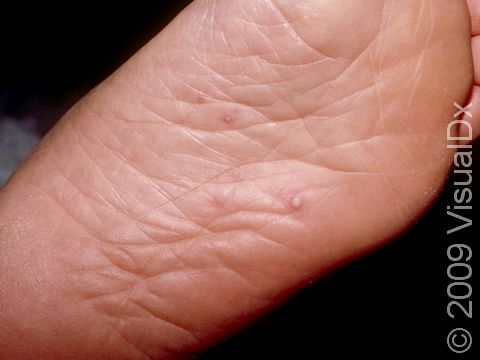
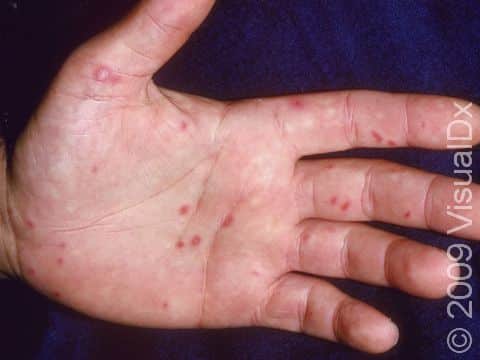
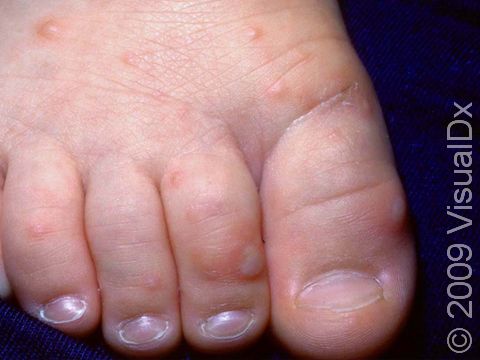
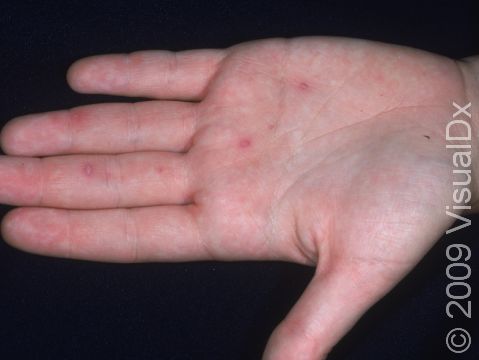
Initially, red macules (small, smooth, flat spots) develop in the lining of the mouth and on the tongue, gums, and/or throat, which develop into vesicles (small fluid-filled bumps) and rapidly form erosions (open sores). Then, oval or football-shaped blisters surrounded by a red ring appear on the hands, feet, and groin. These may be painful. Lesions on the hands and feet typically appear on the sides and backs of the fingers and toes. The palms and soles may also be affected.
After about a week, the rash will go away and your child will start to feel better.
Self-Care Guidelines
Hand, foot, and mouth disease is a self-limited viral infection, meaning it will go away on its own. Treatment is aimed at helping lessen symptoms. Acetaminophen (Tylenol) or ibuprofen (eg, Advil, Motrin) may be used to treat fever and pain. Be sure your child drinks plenty of fluids to stay well hydrated.
To reduce spreading the virus, do not pop the blisters. The virus may be present in a person’s stool for 1 month. Be careful to avoid passing the infection to others by practicing good hygiene. Wash your hands and your child’s hands frequently, particularly after using the bathroom or diaper changes and before eating.
Although most pregnant individuals who become infected with hand, foot, and mouth disease have no symptoms or just a mild illness, the disease can be passed along to a newborn during delivery, which could make the baby very ill. Therefore, anyone infected with hand, foot, and mouth disease should avoid contact with pregnant individuals, particularly those in late pregnancy.
Treatments
Blood tests and procedures to identify the cause of the infection (cultures) are not usually done. However, if your child’s medical professional is concerned that the child might be infected with the bacteria Streptococcus (strep infection), they may perform a throat culture.
Antibiotics do not help treat hand, foot, and mouth disease. Your child’s medical professional will likely recommend that you give the child fluids and something to relieve the pain.
Visit Urgency
See your child’s medical professional if their fever is not brought down by acetaminophen or ibuprofen or if your child has a severe headache, stiff neck, irritability, lethargy, or if they appear very ill.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on May 24th, 2023 at 11:38 am
Not sure what to look for?
Try our new Rash and Skin Condition Finder