Flat Wart
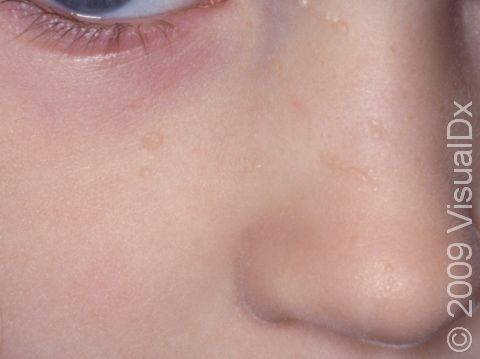
Warts are growths of the skin and inside the mouth that are caused by a virus known as the human papillomavirus (HPV). The virus causes thickening of the top skin layer. Sometimes several flat warts will be in a line from the infant scratching or from combing of the infant’s hair, for example. Flat warts are typically small but can be numerous in a particular area. They will usually go away on their own without any treatment.
Who's At Risk?
Warts can occur in people of all ages and populations, but they are most common in children aged 12-16 years. Infants may acquire warts through a tiny break in their skin if they come into contact with another person (eg, a caregiver or family member) with warts. It is very rare for an infant to develop a wart after touching an object that was handled by another person with warts. However, flat warts may spread more quickly on infants because they often scratch at the warts and may unknowingly cause more warts to form near the same area.
Signs & Symptoms
The most common locations for flat warts include the:
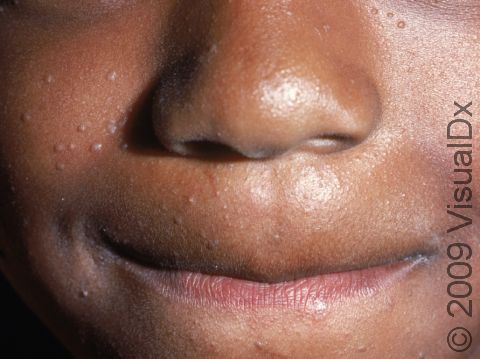
- Face, especially in children.
- Neck.
- Backs of hands.
- Arms.
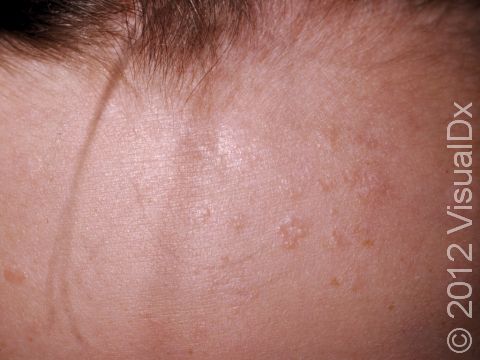
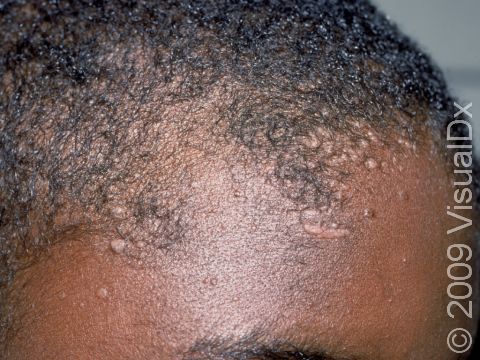
Flat warts are very slightly raised, flat-topped, smooth, round or oval papules (small, solid bumps) ranging in size from 1-3 mm. In lighter skin colors, flat warts may be pink, skin-colored, or yellowish-brown. In darker skin colors, flat warts may be whitish, pink, purple, or brown.
Self-Care Guidelines
Since many warts go away on their own, it is not necessary to treat most warts. Warts also often come back or appear in new areas despite treatment; therefore, it is important to avoid using repeated, painful, or scarring treatments unless the warts are interfering with your child’s daily life.
Before trying any self-care measures, see your baby’s medical professional.
To help reduce the spread of warts, household members should avoid sharing personal items such as towels.
Treatments
If your baby is diagnosed with flat warts, the medical professional may recommend observation only, but in the case of warts that are progressive, application of a topical agent, such as tretinoin, or others, may be recommended.
Visit Urgency
Any baby with warts should be checked by a medical professional.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on November 7th, 2023 at 11:45 am
Not sure what to look for?
Try our new Rash and Skin Condition Finder