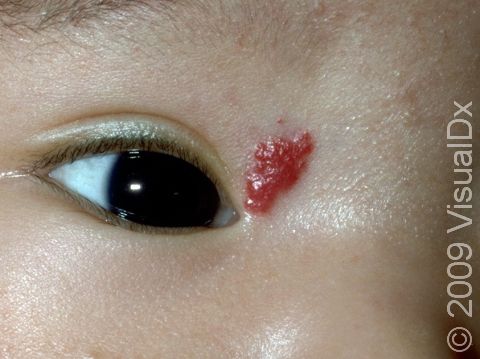
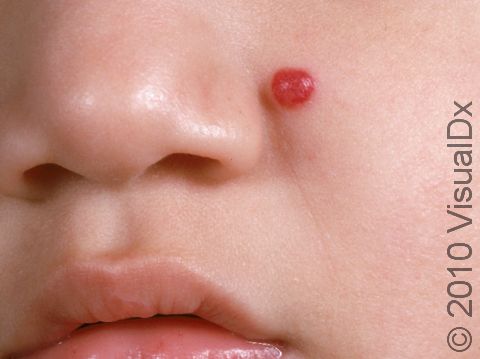
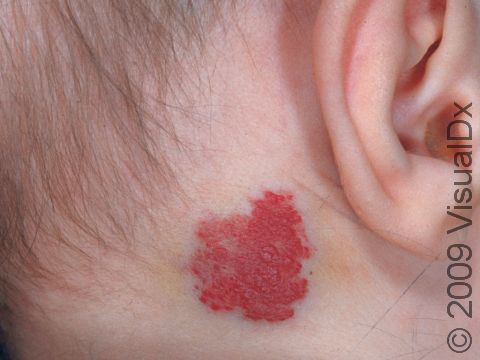
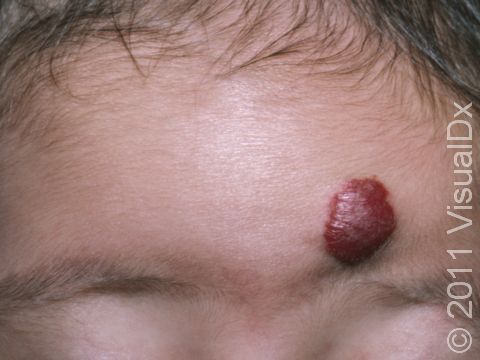
Strawberry Hemangioma (Infantile Hemangioma)
Infantile hemangiomas are common growths of blood vessels that appear shortly after birth and grow rapidly during the first year of life. They usually resolve on their own, shrinking and becoming flatter, over the next few years. Eventually, hemangiomas resolve completely or may leave just some blood vessels or some scarring on the skin. Most hemangiomas only affect the skin, but children with multiple hemangiomas may have associated internal lesions involving the liver, lungs, or other internal organs. These hemangiomas are more serious in nature and usually require close follow-up by your child’s medical professional.
Who's At Risk?
Hemangiomas affect about 10% of infants, and the risk is about 5 times higher in females than males. White infants, premature infants, and low birthweight infants are at an increased risk for hemangiomas.
Signs & Symptoms
Most hemangiomas appear at birth or within the first 2 weeks of life. They may begin as a nodule (raised bump) on the skin or as a reddish patch (a flat, smooth area of skin larger than a thumbnail) that may appear similar to a bruise. They most commonly occur on the head and neck but can occur anywhere on the skin. Hemangiomas grow very rapidly for weeks or months, usually peaking in size at age 6-9 months, and form raised areas ranging in size from a few millimeters to centimeters. They are often bright red with well-defined borders but can be deeper red, maroon, or somewhat purple in color. If a hemangioma grows very large, it may be prone to bleeding spontaneously.
Self-Care Guidelines
If you suspect that your baby has an infantile hemangioma, see their medical professional as they will want to monitor the hemangioma for growth. Applying a thick moisturizer (eg, CeraVe) can help protect the delicate skin and minimize dryness and cracking. If the hemangioma bleeds, treatment with wet compresses and antibacterial ointment can help.
Be sure to watch for signs of infection (such as swelling, redness, warmth, and oozing) for any hemangiomas that bleed.
Treatments
For smaller lesions, a topical treatment (such as timolol) may be used. Laser treatment may be recommended for flatter, small lesions. A steroid injection or an oral medication (propranolol) may also be recommended. For larger hemangiomas or those that are close to important anatomic structures, oral propranolol or oral steroids may be used. Later on, after treatment, laser therapy may be used for any residual color, and sometimes surgery is needed if there is a scar that remains.
Visit Urgency
Seek medical care if your baby’s hemangioma is large or growing, if it changes in color, starts to bleed, appears infected, or appears to be blocking their vision, breathing, or feeding. Also seek medical care if the hemangioma is in a cosmetically sensitive location, such as the face. Hemangiomas that are located in the diaper area or on the lower lip are particularly prone to bleeding, due to friction.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 17th, 2024 at 2:46 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder