Genital Wart (Condyloma Acuminatum)
Genital warts (condyloma acuminata) are caused by the wart virus human papillomavirus (HPV), of which there are over 100 different strains. Subtype numbers 6 and 11 cause 90% of genital warts and are considered low risk because they very rarely cause genital or anal cancer. But subtypes 16 and 18, for example, are considered high risk because, although they rarely cause genital warts, they can lead to cervical or anal precancer and cancer.
HPV is spread by skin-to-skin contact during sexual activity, and there does not need to be vaginal or anal intercourse to spread the infection.
Most people who become infected with HPV will not have symptoms and will clear the infection on their own. For people who do develop genital warts, there are many options for treatment, all of which are meant to remove the visible warts.
Who's At Risk?
Genital warts are the most common sexually transmitted infection (STI) and affect millions of people throughout the world. Approximately 15% of the US population is infected with HPV.
HPV infection occurs in people of all ages and sexes. The risk of acquiring the virus is higher in those who have had many sexual partners and those who had sexual intercourse for the first time at a young age.
More than 50% of girls will get HPV within 2 years of becoming sexually active. It is estimated that 75%-80% of sexually active men and women will be infected with HPV at some point in their lives.
Signs & Symptoms
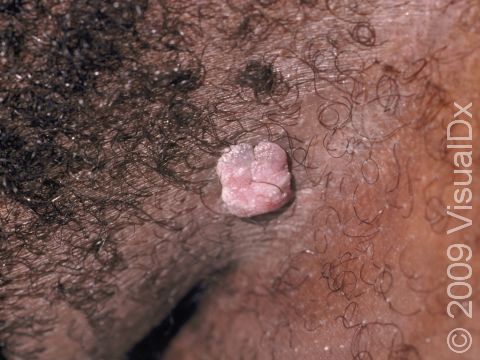
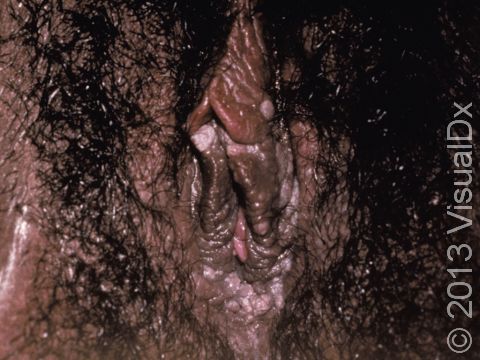
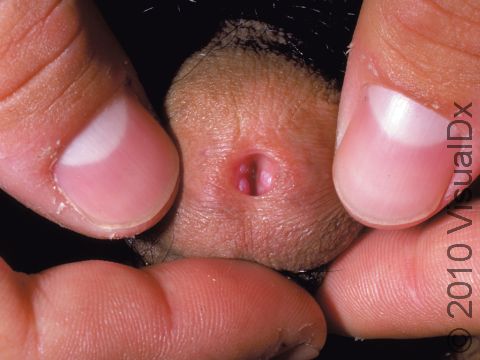
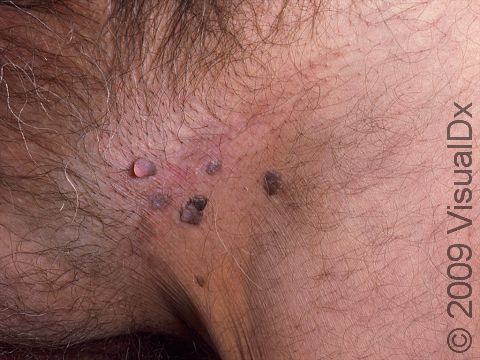
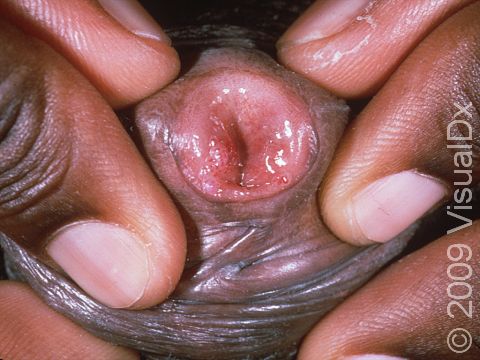
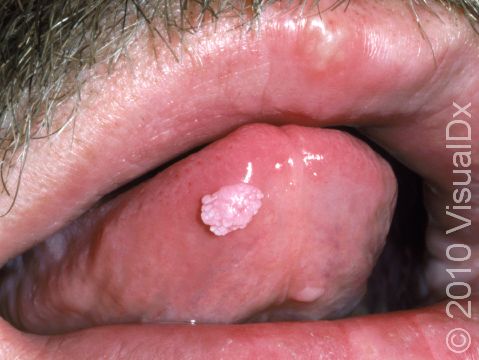
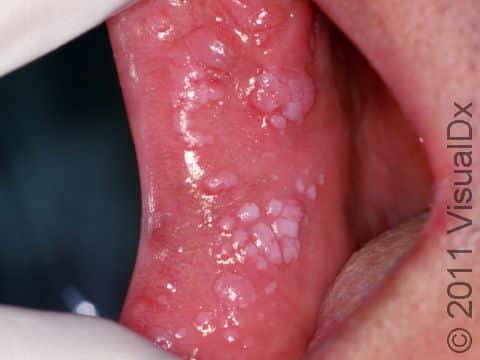
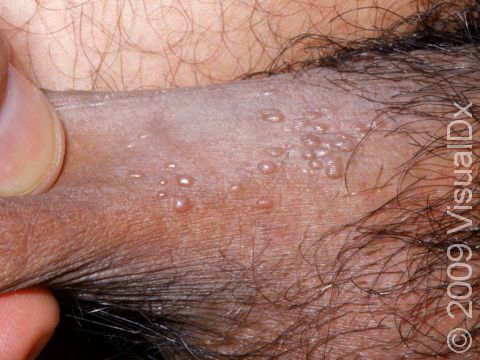
Genital warts may be smooth and flat or bumpy, or they can look cauliflower-like with a small stalk. They can be pink, red, white, grayish, or brown. Most genital warts are very small, but several warts can group together, forming a plaque (an area larger than a thumbnail).
Genital warts can be seen on the labia, vagina, penis, scrotum, anus, skin around the anus, and urethra. Genital warts usually do not have any symptoms associated with them, although the warts can bleed and become painful with intercourse if they are located within the vagina.
Self-Care Guidelines
You can decrease your risk of getting genital warts by using condoms and by having few sexual partners or by abstaining from sexual activity. Unfortunately, condoms do not completely protect against HPV, and an infected person can spread the virus even if they do not have any visible warts.
Gardasil-9 (9vHPV), a US Food and Drug Administration (FDA)-approved vaccine for HPV, is available and protects against 9 types of HPV, including high-risk strains 16 and 18 that cause most HPV cancers as well as low-risk strains that cause most genital warts. In the United States, Gardasil is approved for girls / women and boys / men aged 9-45. The vaccine is most effective when given before an individual becomes sexually active, but it can be given after sexual activity has begun.
Treatments
The goal of genital wart treatment is to remove visible warts and decrease the risk of spreading the virus. There are many different treatments your medical professional may recommend, none of which are 100% effective. Most treatment types will get rid of the warts in 60%-90% of cases, however.
Some prescription treatments are applied by the patient. These include:
- Imiquimod 3.75% cream (Zyclara) – Imiquimod works by boosting your immune system to kill the virus. This medication may weaken condoms, and you should avoid sexual activity while the cream is on your skin. Do not use imiquimod during pregnancy.
- Imiquimod 5% cream (Aldara).
- Podofilox (podophyllotoxin) 0.5% gel or solution (Condylox) – This should not be used during pregnancy.
- Other possible treatments include sinecatechins 15% ointment, 5-fluorouracil 5% cream, cidofovir 1% gel, retinoids, and sodium nitrite 6% with citric acid 9%.
Treatments performed by a medical professional include:
- Podophyllin resin, 15%-25% solution – This should not be used during pregnancy.
- Trichloroacetic acid.
- Cryotherapy – Liquid nitrogen is used to freeze the warts.
- Surgical removal – This may need to be performed by a specialist with local anesthesia and is usually for instances where there are several warts.
- Laser treatment – Carbon dioxide laser treatment is useful in instances where there are several urethral or vaginal warts.
Most of these treatments require multiple applications, and different medications may be needed. Common side effects of all treatments include skin irritation and redness. Some people may also develop scars at the sites of the warts.
Your medical professional may also recommend testing for other STIs, such as gonorrhea, syphilis, HIV, hepatitis, and chlamydia.
Visit Urgency
Do not attempt self-care if you suspect you might have genital warts. See your medical professional for treatment to remove the warts and to reduce the chances of passing the virus to your partner. Also, if your partner has been diagnosed with genital warts, you should be checked for HPV infection.
For women, it is important to have routine pelvic exams, which may include a Papanicolaou test (commonly called a Pap smear) to look for any signs of abnormal cervical cells, which can be the first sign of cervical cancer.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
Centers for Disease Control and Prevention. Human papillomavirus (HPV) vaccination: What everyone should know. CDC. https://www.cdc.gov/vaccines/vpd/hpv/public/. Updated 2021 Nov 16.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on January 8th, 2026 at 12:50 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder